Comparing clinical presentation and interventions for upper extremity
Contrasting shoulder conditions
- Glenohumeral dislocations and instability
- Dislocations of the glenohumeral joint caused by traumatic or atraumatic reasons
- Trauma is due to direct injury, most commonly a fall on an outstretched hand (FOOSH) mechanism of injury
- Atraumatic can be due to repetitive injury, causing hypermobility
- Types of dislocations:
- Anterior-inferior dislocations: Most common type (95%). Mechanism is a combination of motions including: excessive horizontal abduction, abduction, external (lateral) rotation, and extension/hyperextension of the upper extremity.
-
If traumatic can lead to: Disruption anterior glenohumeral/capsular ligament, subscapularis, and anterior/inferior glenoid labrum Sulcus sign: a depression or groove appears between the acromion and the humeral head.
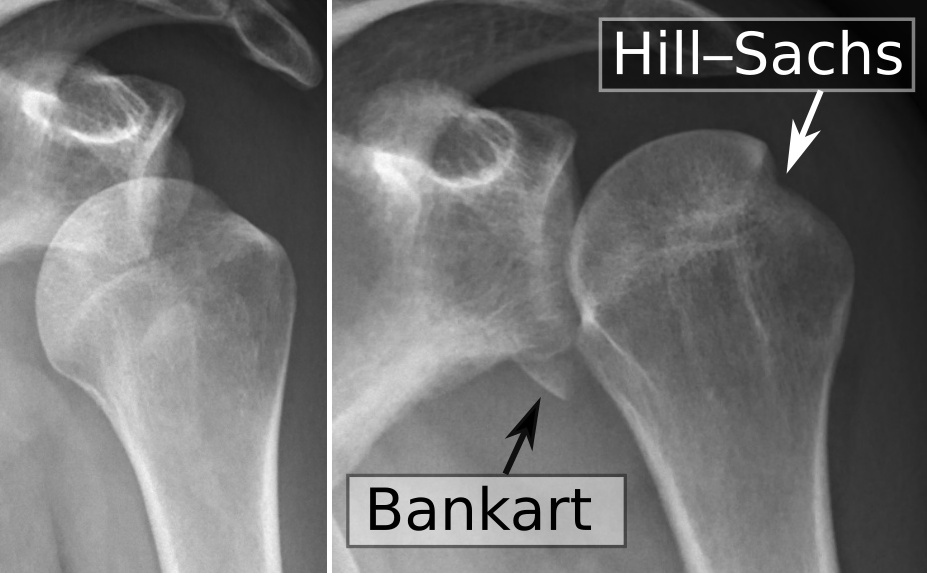
- Hills-Sachs lesion: compression fracture of the posterior humeral head
- Bankart lesion: avulsion of the anterior-inferior glenoid labrum
- Axillary nerve injury: numbness, tingling, and weakness in the deltoid
-
- Anterior-inferior dislocations: Most common type (95%). Mechanism is a combination of motions including: excessive horizontal abduction, abduction, external (lateral) rotation, and extension/hyperextension of the upper extremity.
- Dislocations of the glenohumeral joint caused by traumatic or atraumatic reasons
- Posterior dislocations: rare, caused by horizontal adduction and internal rotation
- Symptoms
- Popping during movements
- Repeated dislocations or subluxations of the glenohumeral joint
- Diagnosis
- Clinical presentation — Sulcus sign
- Special test — apprehension test (Gold Standard)
- X-ray
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Surgery as indicated
- Physical therapy interventions
- Strengthening the capsule and muscles directly connected to prevent further dislocations
- Functional training
- Avoidance of apprehension position
- Surgical protocols if indicated
- With anticipated return to function in 3-4 months
- Labral tears
-
Tear in the cartilage ring that surrounds the shoulder joint; divided into above the middle of the socket and below the middle of the socket
- Above the middle of the socket is called a SLAP (superior labral anterior-posterior) tear; can also involve the biceps tendon
- Below the middle of the socket is called a Bankart lesion; it can also involve an avulsion fracture of the anterior/inferior lip of the glenoid (bony Bankart)
-
Labral tears are associated with traumatic injury or repetitive shoulder dislocations
-
- Symptoms:
- Pain increased with overhead movement or behind the back
- Shoulder weakness
- Shoulder instability/dislocation
- Pain with resisted flexion of the biceps
- Tenderness over the anterior shoulder
- Diagnosis
- Clinical presentation
- MRI
- Arthroscopic surgery — gold standard for diagnosis
- Medical Interventions
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Surgery if indicated
- Physical therapy interventions
- Focus on return to function without pain
- Restoration of muscle imbalances
- Address underlying causes of labral tears
- Surgical protocols if indicated
- With anticipated return to function in 3-4 months
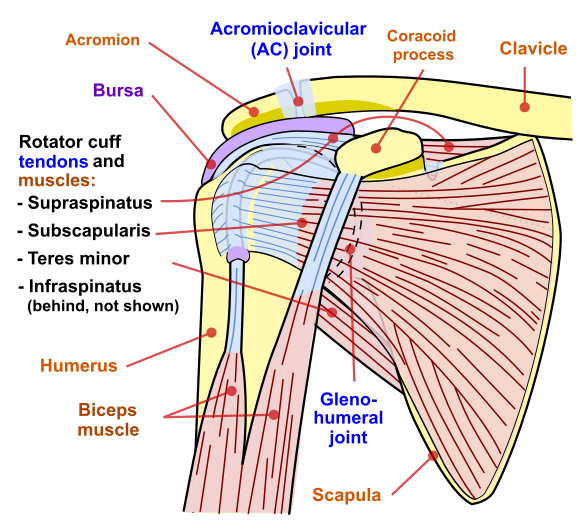
- Rotator cuff tendonitis
- Caused by mechanical impingement of the distal attachment of the rotator cuff, causing inflammation of the tendons
- Increased risk for development of tendonitis due to poor vascularity at attachment sites
- Caused by mechanical impingement of the distal attachment of the rotator cuff, causing inflammation of the tendons
- Impingement syndrome
- Impingement (entrapment) of the rotator cuff tendon against the acromion due to mechanical repetition
- Symptoms
- Pain in the anterior and superior aspect of the shoulder
- Pain and weakness that worsen with overhead movements, such as reaching, throwing, or lifting objects
- Pain that may radiate down the arm
- Pain that is worse at night
- Diagnosis and pain referral location
- Clinical presentation
- Special tests
- Hawkins-Kennedy - Sub acromial region
- Neer’s Superior coracho-acromial region
- Painful arc (Shoulder pain that occurs when abducting an arm between 70 and 120 degrees).
- Shoulder pain that occurs when abducting an arm between 70 and 120 degrees.
- MRI
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Surgery if indicated
- Physical therapy intervention
- Avoidance of shoulder elevation greater than 90 degrees to avoid subacromial compression — acute phase
- Postural re-education — improve forward head, rounded shoulders, and kyphotic posture (Upper cross syndrome)
- Correction of muscle imbalances
- Improve joint mobility
- Return to previous functional status
- Surgical decompression if indicated
- Rotator cuff tear/damage
- Causes acute tear from a fall on an outstretched hand (FOOSH), sudden heavy lifting, or the shoulder in an awkward position
- Partial and degenerative damage from an increased risk for the development of tendonitis due to poor vascularity at attachment sites
- Symptoms
- Pain when raising or lowering the arm
- Pain when reaching behind your back
- Pain that worsens after lying down on the affected side
- Pain that is worse at night
- Diagnosis
- Clinical presentation
- Special tests — empty can test, drop arm test, manual muscle testing of infraspinatus and supraspinatus
- MRI
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Surgery if indicated
- Physical therapy intervention
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Surgical protocols if indicated
- Subacromial/subdeltoid bursitis
- Subacromial and subdeltoid bursae become inflamed (close relationship with rotator cuff tendonitis )
- The bursa becomes trapped (impinged) beneath the acromion arch
- Subacromial and subdeltoid bursae become inflamed (close relationship with rotator cuff tendonitis )
-
Symptoms
- Pain may worsen with overhead movements, such as reaching for objects or lifting the arm.
- The shoulder may be tender to the touch, especially around the acromion process.
- The bursa may become inflamed and swollen, causing a visible bulge or lump in the shoulder.
- The shoulder may feel stiff and difficult to move
- When moving the shoulder, there may be clicking or popping sounds as the bursa rubs against the acromion bone.
- Empty end-feel joints’ passive movement stops due to the patient’s pain, not because of a physical blockage
-
Diagnosis:
- Clinical examination - ruling in and out other diagnoses based on symptomatology, as well as assessment of range of motion and muscle strength
-
Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
-
Physical therapy management
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Bicipital tendonitis
- Inflammation of the long head of the biceps
- Cases can be mechanical trapping (impingement) of the long head of the biceps between the acromion and the bicipital groove of the humerus
- Inflammation of the long head of the biceps
- Symptoms
- Sharp, throbbing, or dull pain in the front of the shoulder that may radiate down the upper arm — pain worsens with overhead movements, such as reaching, lifting, or throwing.
- Localized tenderness over the biceps tendon, particularly where it passes over the shoulder joint.
- A feeling or sound of snapping or popping in the shoulder when moving the arm.
- Weakness in the biceps muscle, making it difficult to lift or bend the arm.
- Diagnosis
- Clinical presentation, positive Speed’s, Yergason, and biceps load II test.
- MRI
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Physical therapy management
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Adhesive capsulitis
- Restriction in shoulder motion due to inflammation of the joint capsule
- Restrictions are in external rotation (greatest), abduction, and flexion (capsular pattern of the shoulder)
- Reason for diagnosis can be repetitive motion, diabetes, cardiovascular disease, or thyroid disease
- Restriction in shoulder motion due to inflammation of the joint capsule
- Symptoms
- Restriction in external rotation, abduction, and flexion, causing functional deficits
- Diagnosis
- Clinical presentation
- Functional limitations
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Management of diabetes, cardiovascular, or thyroid disease if applicable
- Physical therapy management
- Improve joint mobility in the capsular pattern
- Return to prior functional status
- Improve muscle imbalances
- Acromioclavicular and sternoclavicular disorders
- Occurs when falling on the adducted shoulder or when in collision with another individual, particularly during a sporting event
- Grades of injury
- Type I
- A minor sprain of the acromioclavicular ligament
- No radiographic displacement
- No tear of the acromioclavicular or coracoclavicular ligament
- Type II
- A tear of the acromioclavicular ligament, but not the coracoclavicular ligaments
- Less than 25% increase in the coracoclavicular interspace
- Type III
- Tears of both the acromioclavicular and coracoclavicular ligaments
- 25% to 100% displacement of the clavicle
- Type IV
- Tears of both the acromioclavicular and coracoclavicular ligaments
- Posterior displacement of the distal clavicle into the trapezius fascia
- Type I
- Grades of injury
- Occurs when falling on the adducted shoulder or when in collision with another individual, particularly during a sporting event
- Symptoms:
- Pain at the top of the shoulder, which may worsen when moving the arm
- Swelling, bruising, or tenderness over the joint
- Limited range of motion in the shoulder
- A bump or deformity where the clavicle or scapula has moved
- A crunching or grinding sound when moving the arm
- The collarbone may appear to move upward
- The shoulder may appear to droop
- Diagnosis
- Clinical presentation
- Subjective statement of the mechanism of injury
- X-ray
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Surgery is rare due to the increased risk of deterioration it can have on the AC joint
- Physical therapy management
- Sling during the acute phase to avoid shoulder elevation
- Functional training and strengthening of muscles surrounding the joint
- Manual therapy to the acromioclavicular or coracoclavicular ligament as appropriate
- Proximal humeral fracture
- Occurs due to a fall on an outstretched arm and motor vehicle accident
- Stable fractures that do not require surgery
- Occurs due to a fall on an outstretched arm and motor vehicle accident
- Symptoms
- Intense shoulder pain
- Swelling and bruising
- Difficulty moving the arm
- Diagnosis:
- Clinical presentation
- Subjective statement
- X-ray
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Physical therapy interventions
- Early passive range of motion to decrease range of motion restrictions
- Non-weight-bearing early per physician recommendations
- Eventual active range of motion, strengthening, and coordination activities initiated once medically cleared
- Distal humeral fracture
- Trauma causes a fracture at the distal humerus
- Immediate attention must be given to whether a supracondylar fracture is due to the increased likelihood of neurovascular involvement
-
Radial nerve involvement associated with posterior type injuries may lead to damage of vascular structures, pulselessness, and/or paralysis
-
Ulnar nerve involvement associated with flexion type injuries may lead to paralysis and a loss of fine motor control in the hand
-
In children, it can cause malunion due to growth plate involvement
-
- Lateral epicondyle fractures will require internal fixation (rod and screws implanted in arm) for adults, percutaneous removal pins for non-skeletally mature fractures, for proper alignment
- Immediate attention must be given to whether a supracondylar fracture is due to the increased likelihood of neurovascular involvement
- Trauma causes a fracture at the distal humerus
- Symptoms
- Severe pain in the elbow area that may radiate to the forearm and shoulder.
- Pronounced swelling around the elbow joint.
- The elbow may appear bent or twisted.
- Diagnosis
- Clinical presentation
- X-ray
- Medical management
- Surgery for internal fixation
- Acetaminophen or non-steroidal anti-inflammatory (NSAIDs)
- Physical therapy management
- Aid in the management of symptoms during the inflammatory phase
- After surgical intervention and the time of immobilization has concluded, we will begin with mobility and strengthening
- Thoracic outlet syndrome
- Compression of the neurovascular bundle that includes the brachial plexus, sympathetic trunk, subclavian artery and vein, and phrenic and vagus nerves due to alteration in thoracic outlet size
- Common areas of compression are:
- Superior thoracic outlet
- Scalene triangle
- Between the clavicle and the first rib
- Between the pectoralis minor and the thoracic wall
- Symptoms
- Pain in the neck, shoulder, arm, or hand
- Pain that worsens with certain activities, such as overhead reaching or holding objects
- Numbness, tingling, or burning sensations in the arm, hand, or fingers
- Symptoms may be worse at night or after prolonged activity
- Weakness in the arm, hand, or grip
- Swelling in the arm or hand,
- Coldness or cyanosis in the fingers
- Diagnosis
- Clinical examination
- Special tests
- Adson’s test
- Roos test
- Wright test
- Costoclavicular test
- Special tests
- X-ray
- MRI
- Clinical examination
- Medical management
- Acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs)
- Surgical removal of cervical rib as indicated
- Surgical release of the scalenes as indicated
- Physical therapy management
- Interventions vary based on the cause of thoracic outlet syndrome
- Postural re-education
- Joint mobility and strengthening as appropriate
Contrasting elbow conditions
- Medial epicondylitis
- Inflammation of the pronator teres and the flexor carpi radialis tendons at the attachment of the medial epicondyle
- Typically due to overuse in activities that require excessive pronation at the forearm
- Commonly referred to as golfer’s elbow
- Typically due to overuse in activities that require excessive pronation at the forearm
- Inflammation of the pronator teres and the flexor carpi radialis tendons at the attachment of the medial epicondyle
- Symptoms
- Pain on the inner side of the elbow, often radiating down the forearm
- Pain that worsens with activities that involve gripping, twisting, or bending the wrist
- Tenderness to the touch on the medial epicondyle
- Weakness in the grip
- Numbness or tingling in the ring and little fingers
- Stiffness in the elbow
- Diagnosis
- Clinical presentation
- Special test
- Mill’s test
- Special test
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Bracing may be indicated
- Lateral epicondylitis
- Inflammation of the extensor carpi radialis brevis tendon at its attachment to the lateral epicondyle
- Gradual onset occurring with repetitive wrist extension, resulting in overloading of the extensor carpi radialis
- Inflammation of the extensor carpi radialis brevis tendon at its attachment to the lateral epicondyle
- Symptoms
- Gradual onset of pain on the outer side of the elbow, often worse with gripping, twisting, or extending the wrist
- Localized tenderness over the lateral epicondyle
- May be mild swelling around the elbow.
- Pain may spread from the elbow down the forearm or into the wrist.
- Diagnosis
- Clinical presentation
- Special tests
- Cozen’s test
- Special tests
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Bracing may be indicated
- Ulnar collateral ligament injuries
- Due to repetitive valgus stress to the medial elbow, causing stress to the ulnar collateral ligament
- Symptoms
- Pain at the medial elbow at the insertion of the ligament
- Paresthesias in the ulnar nerve distribution in the forearm and hand
- Diagnosis
- Clinical presentation
- Special test
- Tinel test
- Valgus elbow test
- Special test
- MRI
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Determine the phase (acute vs subacute vs chronic) and make an appropriate selection of interventions based on the phase of healing
- Taping may be indicated
- Elbow dislocation
- Caused by trauma to the elbow, causing misalignment from the anatomical position
- Posterior dislocation is the most common
- Posterolateral dislocation occurs as a result of hyperextension from a fall on an outstretched arm
- Posterior dislocations commonly cause an avulsion fracture of the medial epicondyle
- Complete dislocation will impact all of the following structures
- Lateral collateral ligament, anterior capsule, brachialis muscle, wrist flexor muscles, and wrist extensor muscles
- Posterior dislocation is the most common
- Caused by trauma to the elbow, causing misalignment from the anatomical position
- Symptoms
- Intense pain at the elbow joint, especially during movement
- The elbow may appear visibly out of place, with the forearm at an unnatural angle
- The elbow may feel loose or like it is going to give way.
- Difficulty or inability to bend, straighten, or rotate the elbow.
- Swelling and bruising around the elbow joint.
- Diagnosis
- Clinical presentation
- X-ray
- Medical management
- Reduction of dislocation
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Stable elbow (easily reduced and stays in place) — initial immobilization followed by therapy to assist with regaining range of motion and strength
- Unstable elbow (elbow continues to dislocate even after reduction)- surgery indicated
- Nerve entrapments
- Medial nerve entrapment
- Tightness of the pronator teres muscle and under the superficial head of the flexor digitorum superficialis secondary to repetitive gripping activities
- Symptoms
- Pain, numbness, tingling, and weakness in the median nerve distribution in the forearm and below
- Diagnosis
- Clinical presentation
- Manual muscle test of forearm muscles
- Positive Tinel’s test in the median nerve distribution
- Radial nerve entrapment
- Entrapment of the posterior interosseous nerve within the radial tunnel as a result of overhead activities and throwing
- Symptoms
- Lateral elbow pain
- Pain, numbness, tingling, and weakness in the radial nerve distribution in the forearm and below
- Diagnosis
- Clinical presentation
- Manual muscle test of forearm muscles
- Positive Tinel’s test in radial nerve distribution
- Ulnar nerve entrapment
- Compression or trauma at the cubital tunnel, thickened retinaculum, or hypertrophy of the flexor carpi ulnaris muscle
- Symptoms
- Medial elbow pain
- Pain, numbness, tingling, and weakness in the ulnar nerve distribution in the forearm and below
- Diagnosis
- Clinical presentation
- Manual muscle test of forearm muscles
- Positive Tinel’s test in the ulnar nerve distribution
- Medical management for all nerve entrapments
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management for all nerve entrapments
- Early interventions — rest, modalities to reduce inflammation/pain
- Medial nerve entrapment
- Nerve glides for the appropriate nerve
- Median glide
- Sit or stand with your elbow bent and your hand resting on a surface.
- Turn your palm up and spread your fingers wide.
- Gently bend your wrist back towards your forearm.
- Extend your arm out to the side while keeping your wrist bent.
- Turn your palm down and bring your fingers together.
- Repeat these steps several times.
- Radial glide
- Stand or sit with your arms at your sides.
- Turn your palm towards the floor.
- Keep your wrist flexed and your fist clenched.
- Turn your palm towards your body.
- Look over your opposite shoulder.
- Repeat these steps several times.
- Ulnar glide
- Stand or sit with your arms at your sides.
- Extend your arm out to the side with your palm facing up.
- Then bend your elbow slightly while rotating your hand outward, simultaneously tilting your head away from the extended arm.
- Repeat several times.
- Night splinting as appropriate
- Functional training
- Patient education
- Median glide
Contrasting conditions of wrist and hand
- Carpal tunnel syndrome
- Compression of the median nerve at the carpal tunnel at the wrist due to inflammation of the wrist flexor tendon or inflammation of the median nerve
- Caused by repetitive wrist motions; other causes may be pregnancy, diabetes, or rheumatoid arthritis
- Compression of the median nerve at the carpal tunnel at the wrist due to inflammation of the wrist flexor tendon or inflammation of the median nerve
- Symptoms
- Numbness and tingling in the thumb, index, and middle fingers
- Pain, often described as burning, aching, or electric shock-like
- Sensitivity to cold or touch
- Weakness in the hand, especially when gripping or making fine movements
- Clumsiness or difficulty with tasks like buttoning clothes or writing
- Dropping objects
- Diagnosis
- Clinical presentation
- Special tests
- Tinel’s,
- Phalen’s
- Special tests
- Electrodiagnostic testing — tests if a nerve signal is moving and its speed
- Clinical presentation
- Medical management
- Acetaminophen or non — steroidal anti-inflammatory (NSAIDs)
- Physical therapy management
- Range of motion, strengthening
- Corrections of biomechanical causes
- Functional exercises
- Bracing is the most appropriate option during pregnancy
- deQuervain’s tenosynovitis
- Inflammation of the extensor pollicis brevis and abductor pollicis longus
- Due to repetitive microtrauma o,r occur during pregnancy
- Inflammation of the extensor pollicis brevis and abductor pollicis longus
- Symptoms
- Pain at the base of the thumb that radiates into the forearm.
- Swelling and tenderness on the thumb side of the wrist.
- A feeling of catching or snapping when moving the thumb or wrist.
- Pain or stiffness when grasping, pinching, or extending the thumb.
- Difficulty gripping or holding objects.
- Numbness or tingling in the thumb or index finger.
- Diagnosis
- Clinical presentation
- Special tests-
- Finkelstein’s test
- WHAT
- Special tests-
- MRI
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Range of motion, strengthening
- Corrections of biomechanical causes
- Functional exercises
- Bracing is the most appropriate option during pregnancy
- Colles fracture
- Fracture causing posterior displacement of the distal radius with radial shift of the wrist and hand
- Most common fracture from falling on an outstretched hand with the wrist in extension and radial deviation.
- Can cause median nerve damage if edema is unmanaged
- Fracture causing posterior displacement of the distal radius with radial shift of the wrist and hand
- Symptoms
- Sharp, immediate pain, especially when bending or gripping the wrist.
- Pronounced swelling and bruising around the wrist.
- The wrist may appear bent or crooked, often resembling a “dinner fork”.
- Diagnosis
- Clinical presentation
- X-ray
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Immobilization for 5-8 weeks n a position opposite the injury, wrist flexion and ulnar deviation
- Physical therapy management
- After removal of the cast
- Range of motion, gaining wrist extension is most important before strengthening
- Pain, edema control
- Use of modalities as appropriate
- Functional exercises
- After removal of the cast
- Scaphoid fracture
- Due to falling onto an outstretched hand
- This is the most common fractured carpal bone
- Due to falling onto an outstretched hand
- Symptoms
- Pain located in the anatomical snuff box and weakness on the thumb side of the wrist, especially when gripping or pinching objects.
- Diagnosis
- Clinical presentation
- Diagnosis of rule-out
- X-ray
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Immobilization for 6-8 weeks due to poor blood supply to this bone
- Physical therapy management
- Before cast removal
- Range of motion exercises to proximal and distal joints, the scaphoid, to maintain pre-injury flexibility
- After removal of the cast
- Range of motion, strengthening
- Pain, edema control
- Use of modalities as appropriate
- Functional exercises
- Before cast removal
- Dupuytren’s contracture
- Contracture of the palmar fascia leading to flexion of the digits towards the palm
- Common in the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints of the fourth and fifth digits in non-diabetic and the third and fourth in diabetic
- Contracture of the palmar fascia leading to flexion of the digits towards the palm
-
Symptoms
- Small, hard lumps in the palm, often near the base of the ring or little finger.
- Thickened bands of tissue that run from the nodules to the fingers.
- The affected fingers are gradually pulled into a bent position, making it difficult to straighten them out.
-
Diagnosis
- Clinical presentation
-
Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Wound care may be indicated
- Surgery may be indicated
-
Physical therapy management
- Splinting
- Flexibility exercises
- Restoration of normal hand function
:::
-
Boutonnière deformity
- Rupture of the central tendon slip of the extensor hood
- Commonly occurs after trauma to the hand or with the diagnosis of rheumatoid arthritis
- Deformity noted is extension of MCP and DIP with flexion of PIP
- Rupture of the central tendon slip of the extensor hood
- Symptoms
- Deformity as noted above
- Diagnosis
- Clinical presentation
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Management of rheumatoid arthritis
- Physical therapy management
- Splinting
- Taping
- Flexibility exercises
- Swan neck deformity
- Contracture of intrinsic muscles with dorsal subluxation of lateral extensor tendons
- Commonly occurs after trauma to the hand or with the diagnosis of rheumatoid arthritis
- Deformity noted is flexion of the MCP and DIP with hyperextension of the PIP
- Contracture of intrinsic muscles with dorsal subluxation of lateral extensor tendons
- Symptoms
- Deformity as noted above
- Diagnosis
- Clinical presentation
- Possibly x-ray imaging (rarely used)
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Management of rheumatoid arthritis
- Physical therapy management
- Splinting
- Taping
- Flexibility exercises
- Mallet finger
- Rupture or avulsion of the extensor tendon at its insertion into the distal phalanx digit
- Commonly occurs after trauma, forcing the distal phalanx into a flexed position
- Deformity noted is flexion of the DIP
- Rupture or avulsion of the extensor tendon at its insertion into the distal phalanx digit
- Symptoms
- Deformity as noted above
- Diagnosis
- Clinical presentation
- Possible MRI (rarely used)
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Splinting
- Taping
- Flexibility exercises
- Ape hand deformity
- Median nerve dysfunction causes thenar muscle weakness with the first digit moving dorsally until it becomes aligned with the second digit
- Symptoms
- Inability to move the thumb in and out of the palm
- Inability to oppose the thumb
- Limited ability to flex and extend the thumb
- Sensory loss or tingling in the thumb
- Weakened forearm pronation
- Weakened finger flexion
- Diagnosis
- Clinical presentation
- Electrodiagnostics
- Medical management
- Acetaminophen or non-steroidal inflammatory (NSAIDs)
- Physical therapy management
- Splinting
- Taping
- Flexibility exercises
- Functional strengthening and coordination activities