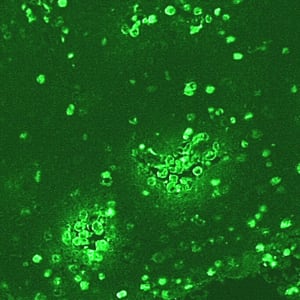
Naegleria fowleri
Naegleria fowleri
Commonly called the “brain-eating amoeba.” This free-living amoeba is found in warm freshwater (e.g., lakes, rivers, and hot springs) and in soil.
Transmission and pathogenesis
It typically enters through the nose after swimming or diving in contaminated lakes and rivers. Rarely, it has been associated with neti pot (a small pot used for nasal rinsing) use, because tap water may be contaminated.
After entering the nose, the amoeba migrates to the brain via the olfactory nerve.
Clinical disease
It causes PAM (primary amoebic meningoencephalitis), which presents with:
- Fever, headache, nausea, vomiting
- Followed by neck stiffness, seizures, altered consciousness, and coma
Only 5 cases so far have survived the infection in North America.
Laboratory diagnosis
PAM and Naegleria fowleri infection can be diagnosed in the laboratory by:
- Detecting organisms in cerebrospinal fluid (CSF), biopsy, or tissue specimens
- Nucleic acid detection in CSF, biopsy, or tissue specimens
- Detection of antigen in CSF, biopsy, or tissue specimens
Motile amoebae can often be seen moving rapidly under a microscope when examining a fresh CSF sample. The amebae can also be stained with a variety of stains, such as Giemsa-Wright or a modified trichrome stain. Culture can be done as co-culture with E.coli.
IIF of Naegleria fowleri in brain tissue, viewed under UV microscopy.