Male reproductive system
The male reproductive system includes the testes, which produce sperm. Sperm are then transported through the epididymis, ductus deferens, ejaculatory ducts, and urethra. The system also includes accessory glands (the seminal vesicles, prostate, and bulbourethral glands). Their secretions contribute essential components of semen and support reproduction.
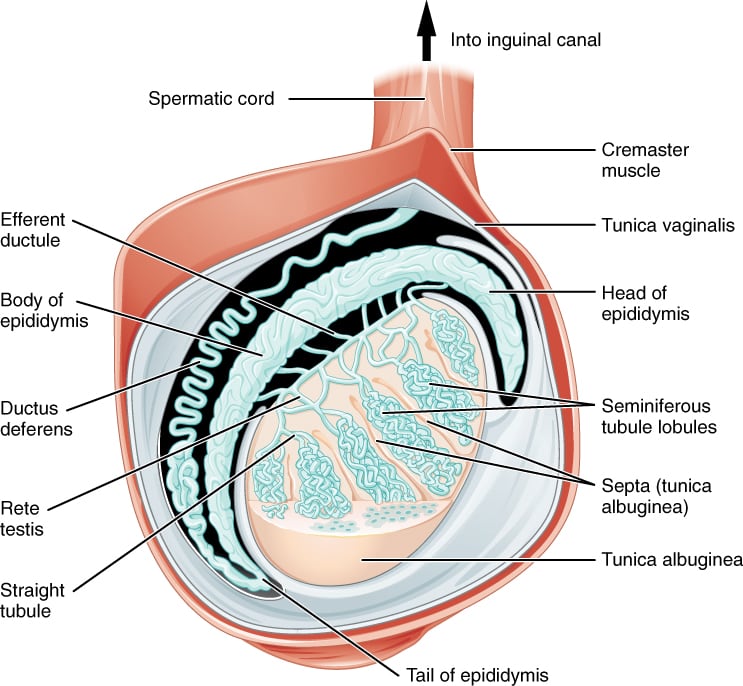
Testes
The testes are the male gonads. They lie in the scrotum and are suspended by the spermatic cord and dartos muscle. Each testis is surrounded by:
- An outer tunica vaginalis (with visceral and parietal layers)
- An inner, tough tunica albuginea
Septa from the tunica albuginea divide the testes into about 300 lobules. Each lobule contains 1-4 tightly coiled seminiferous tubules, which are the site of spermatogenesis.
The seminiferous tubules are lined by germinal epithelium and contain two key cell types: Sertoli cells and spermatogenic (germ) cells. Spermatozoa are released into the lumen of the seminiferous tubules.
-
Sertoli cells: Sertoli cells are elongated columnar cells with characteristic ruffled apical and lateral surfaces and oval nuclei. They extend from the basement membrane to the lumen. They surround germ cells and provide nourishment and structural support, which is why they’re also called sustentacular cells. Sertoli cells are joined by tight junctions, forming the blood-testis barrier. They secrete inhibin, mullerian inhibitory factor, and androgen binding protein; phagocytose dying germ cells and excess cytoplasm; and have receptors for FSH.
-
Spermatogenic or Germ cells: These cells undergo spermatogenesis to produce spermatozoa (sperm). Spermatogonia are located basally along the basement membrane and are round, pale or dark, with prominent nucleoli. Primary spermatocytes have granulated nuclei. Spermatids have very little cytoplasm and dark, round nuclei. Dark type A spermatogonia are the source of stem cells, while pale type A spermatogonia differentiate into type B spermatogonia, which then undergo spermatogenesis.
The narrow terminal portions of the seminiferous tubules form the straight tubules (tubuli recti). The straight tubules empty into the rete testes, located posteriorly at a ridge-like structure called the mediastinum of the testis. About 15-20 efferent ductules connect the rete testis to the epididymis. The efferent ductules are lined by ciliated columnar cells and microvilli and are surrounded by a circular layer of smooth muscle.
Leydig cells (interstitial cells) are located in the connective tissue between the seminiferous tubules. They are acidophilic (stain pink with H and E stain) and appear as large polygonal cells with prominent smooth endoplasmic reticulum and highly refractive, rod-shaped cytoplasmic crystals of Reinke. Leydig cells have receptors for LH and secrete testosterone.
The testes are supplied by the testicular arteries, which are branches of the abdominal aorta and run in the spermatic cord. Additional arterial supply comes from the cremasteric branch of the inferior epigastric artery and the artery to the ductus deferens.
Venous drainage occurs through small veins that form the pampiniform plexus in the spermatic cord. This plexus continues as the testicular vein at the deep inguinal ring. The right testicular vein drains into the IVC, while the left testicular vein drains into the left renal vein at a right angle. The right-angle junction and the longer length of the left testicular vein increase the risk of varicoceles on the left.
Lymphatic drainage is to the lateral aortic and pre-aortic nodes. Autonomic nerve supply comes from the tenth and eleventh thoracic spinal nerves through the renal and aortic plexuses.
Epididymis
The epididymis lies along the superior and posterior margins of the testes. Sperm complete their maturation in the epididymis. It connects to the efferent ductules at one end and to the ductus deferens (vas deferens) at the other.
The epididymis is a highly coiled duct with head, body, and tail regions. It is lined by pseudostratified columnar epithelium containing principal cells and basal (stem) cells. Principal cells have well-developed rough endoplasmic reticulum, Golgi apparatus, and characteristic stereocilia. Stereocilia contain actin filaments and increase surface area to support absorption and secretion. The ductus deferens and hair cells of the inner ear are the only other areas to have stereocilia.
The head and body of the epididymis have a circular smooth muscle layer. The tail has inner longitudinal, middle circular, and outer longitudinal layers, which help move sperm toward the ductus deferens.
Ductus deferens or vas deferens
The ductus deferens is a tube-like structure that begins at the inferior pole of the testes and enters the spermatic cord, which passes through the inguinal canal. It dilates at its distal end to form the ampulla and joins the duct of the seminal vesicle to form the ejaculatory duct.
In a vasectomy, the vas deferens is cut and ligated as a form of surgical sterilization. The epithelium and three-layer muscle coat are similar to those of the epididymis.
Ejaculatory ducts
The ejaculatory duct is formed by the joining of the duct from the ampulla of the vas deferens with the duct of the seminal vesicle. It passes through the prostate and opens into the prostatic urethra at the seminal colliculus (verumontanum). It lacks a muscle coat.
Seminal vesicles
The seminal vesicles are paired saccular glands located posterior to the bladder, between the bladder and the rectum. They are the major contributor to seminal fluid. Their secretion contains:
- Fructose (an energy source for sperm)
- Choline
- Prostaglandins (support sperm viability and motility)
- Proteins that coagulate after ejaculation
Their wall contains a muscular coat with an inner circular and outer longitudinal layer, which helps move seminal fluid into the ejaculatory duct during ejaculation.
Semen contains sperm plus secretions from the seminal vesicles, prostate, and bulbourethral glands.