Other neurological conditions
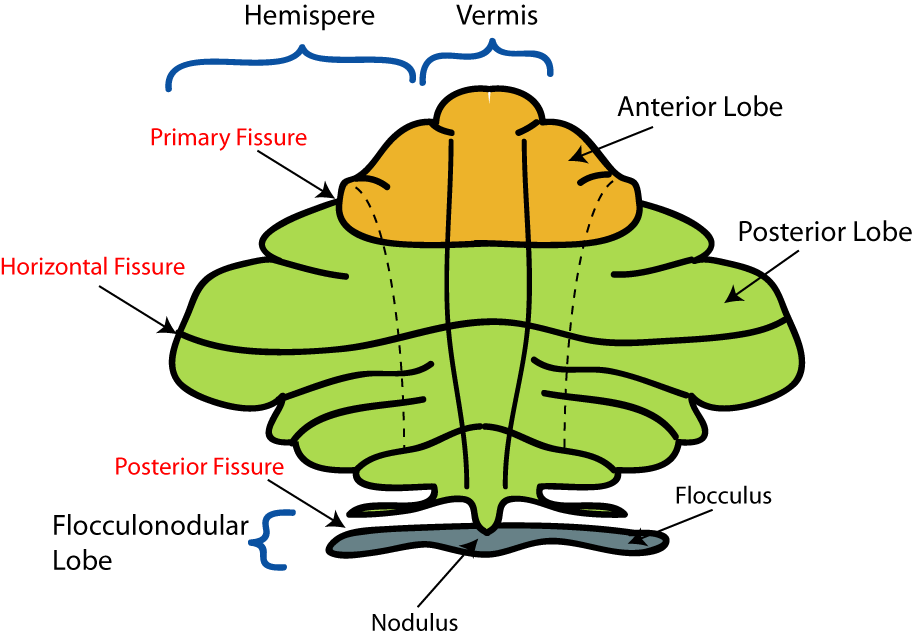
Cerebellar dysfunctions
Common symptoms associated with cerebellum dysfunction:
- Ataxic gait
- Trunk instability
- Intention tremor
- Dysdiadochokinesia
- Dysmetria
- Motor learning impairments
- Cognitive deficits for processing and attention to tasks
- Hypotonia
- Weakness and fatigue
Perception dysfunction
Spatial relation disorders
Types of spatial relation disorders:
- Figure-ground discrimination disorder: inability to perceive an object against a background
- Example: “Where is Waldo” comics
- Spatial relation deficit disorder: inability to properly space objects in relation to one another
- Example: an individual demonstrates difficulty with descriptive terms such as on, over, below, between, under, etc., such as “the book is on the table.”
- Topographical disorientation disorder: inability to navigate a familiar route independently
- Example: an individual with difficulty recalling how many left turns to drive from home to the grocery store
- Depth/distance perception disorder: unable to accurately judge depth or distance
- Example: an individual walking into a wall when ambulating due to an inability to judge distance accurately
- Vertical disorientation disorder: unable to accurately determine what is upright
- Example: an individual sitting or standing quickly while performing head turns can lead to vertical disorientation
Agnosia
Apraxia
2 Common types:
-
Ideomotor Apraxia: difficulty translating the idea of a movement into motor commands. Individuals may struggle to perform tasks such as waving, blowing a kiss, or licking their lips.
-
Ideational Apraxia: inability to plan and sequence complex movements, such as dressing or brushing teeth.
Body scheme/image disorders
Types of body scheme/image disorders
- Body scheme disorder (asomatognosia): inability to recognize a body part as your own
- Example: an individual visualizes having a hand typing, but does not associate the hand as part of their own body
- Visual spatial neglect: ignoring one side of the body and any stimuli from that side
- Example: individuals with stroke who exhibit pusher syndrome
- Right/left discrimination disorder: unable to identify the left and right sides of the body
- Example: an individual asked to step up onto the step with the left but consistently is unable to identify the left lower extremity
- Anosognosia: denial of neglect or lack of awareness of the severity of the dysfunction
- Example: an individual attempts to transfer without assistance, but is a maximum assistant, which leads to injury and is typically in conjunction with a brain injury or an impulsive individual
Encephalitis
Neurological conditions and post- COVID
Trigeminal neuralgia
Symptoms include:
- Sudden, intense pain to one side of the face
- Burning, throbbing, numbness, tingling, or dull aching sensation in between attacks
The pain can be exacerbated by rubbing the cheek (when washing face, shaving, or applying makeup), eating, drinking, talking, blowing nose, brushing teeth, or face interaction with wind. The patient can experience it multiple times per day over a period of time with times of remission.
Two types of trigeminal neuralgia can present:
- Primary: caused by compression of a blood vessel against the trigeminal nerve
- Secondary: caused by stroke, multiple sclerosis, or tumor
Diagnosis is confirmed via clinical examination and imaging. Treatment by physical therapy may include the use of transcutaneous electrical stimulation (TENS) for pain relief and assessment of any other symptoms that may impair function. Medical management may include nerve block, pain medications, and anticonvulsants to treat pain.
Alzheimer’s disease
Symptoms include:
- Sundowning is the first symptom
- Increased confusion/agitation at the time of sunset
- Loss of declarative and procedural memory
- Decreased spatial awareness
- Word finding difficulty
- Changes in personality and behavior
Intervention strategies for individuals with Alzheimer’s disease are as follows:
- Sessions are to assist with maintaining the current level of function
- Basic ADLs and mobility status
- Providing AD and DME as appropriate
- Management of behaviors
- Be consistent in routine (blocked routine)
- Closed environment to minimize distractions
- De-escalate aggressive or combative behaviors by changing the current task
- Re-orient as appropriate