Circulatory system
Functions: circulation of oxygen, nutrients, hormones, ions and fluids, removal of metabolic waste
The circulatory system transports oxygen, nutrients, hormones, ions, and fluids throughout the body and helps remove metabolic waste.
In the lungs, oxygen diffuses into the blood at the alveolar capillaries and binds to hemoglobin in red blood cells. That oxygenated blood then travels to tissues, where cells use oxygen for cellular respiration.
At the same time, carbon dioxide produced by cellular respiration is carried back to the lungs in several forms: it can be converted by carbonic anhydrase into bicarbonate, dissolved in the blood, or bound to hemoglobin and plasma proteins. In the lungs, carbon dioxide diffuses from the blood into the alveoli and is exhaled.
Absorbed nutrients enter the bloodstream from the small intestine. Hormones released by endocrine glands also travel through circulation to reach their target cells.
Fluids and ions in the blood are regulated by the kidney, which reabsorbs water and salt as needed. Urea, a primary waste product, is carried in the blood to the kidneys and excreted in urine.
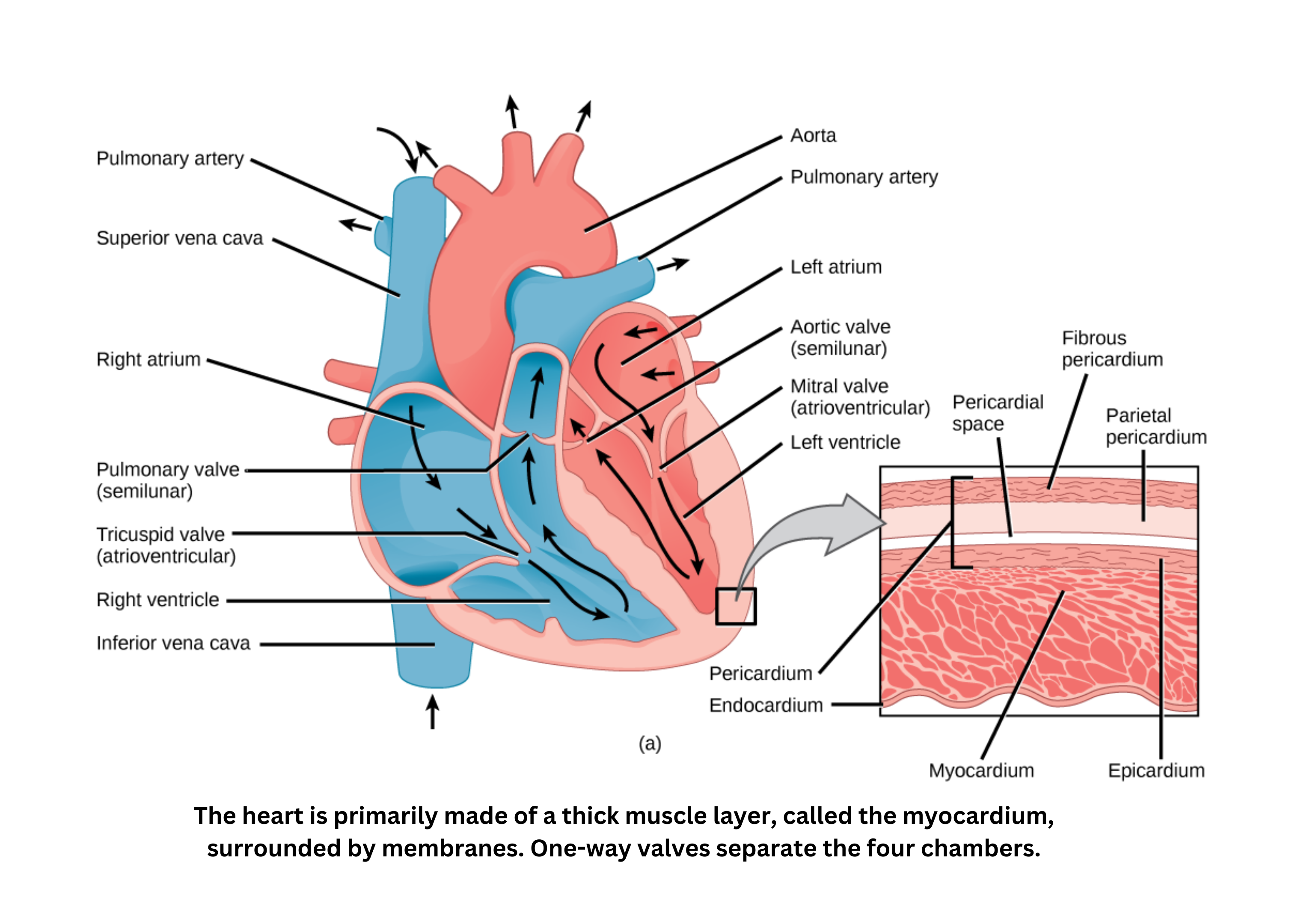
Four-chambered heart: structure and function
A four-chambered heart supports two linked circuits:
- Systemic circulation, which supplies the body with oxygenated blood
- Pulmonary circulation, which sends deoxygenated blood to the lungs for oxygenation
Deoxygenated blood returns via the vena cava to the right atrium, passes through the tricuspid valve into the right ventricle, and flows through the pulmonary valve into the pulmonary artery toward the lungs.
After oxygenation, blood returns through the pulmonary vein to the left atrium, crosses the bicuspid (mitral) valve into the left ventricle, and exits through the aortic valve into the aorta, delivering oxygen-rich blood to the body.
Endothelial cells
Endothelial cells form a single-cell-thick lining throughout all blood vessels. This thin layer supports exchange between the blood and nearby tissues.
Endothelial cells also regulate vascular tone and blood flow by producing both relaxing and contracting agents. These include nitric oxide, various peptides (including endothelin, urotensin, CNP, and adrenomedullin), along with adenosine and other purines.
Although circulating endothelial cells (mature cells shed from blood vessels) are usually present in very low numbers, increased levels often indicate vascular damage in various diseases.
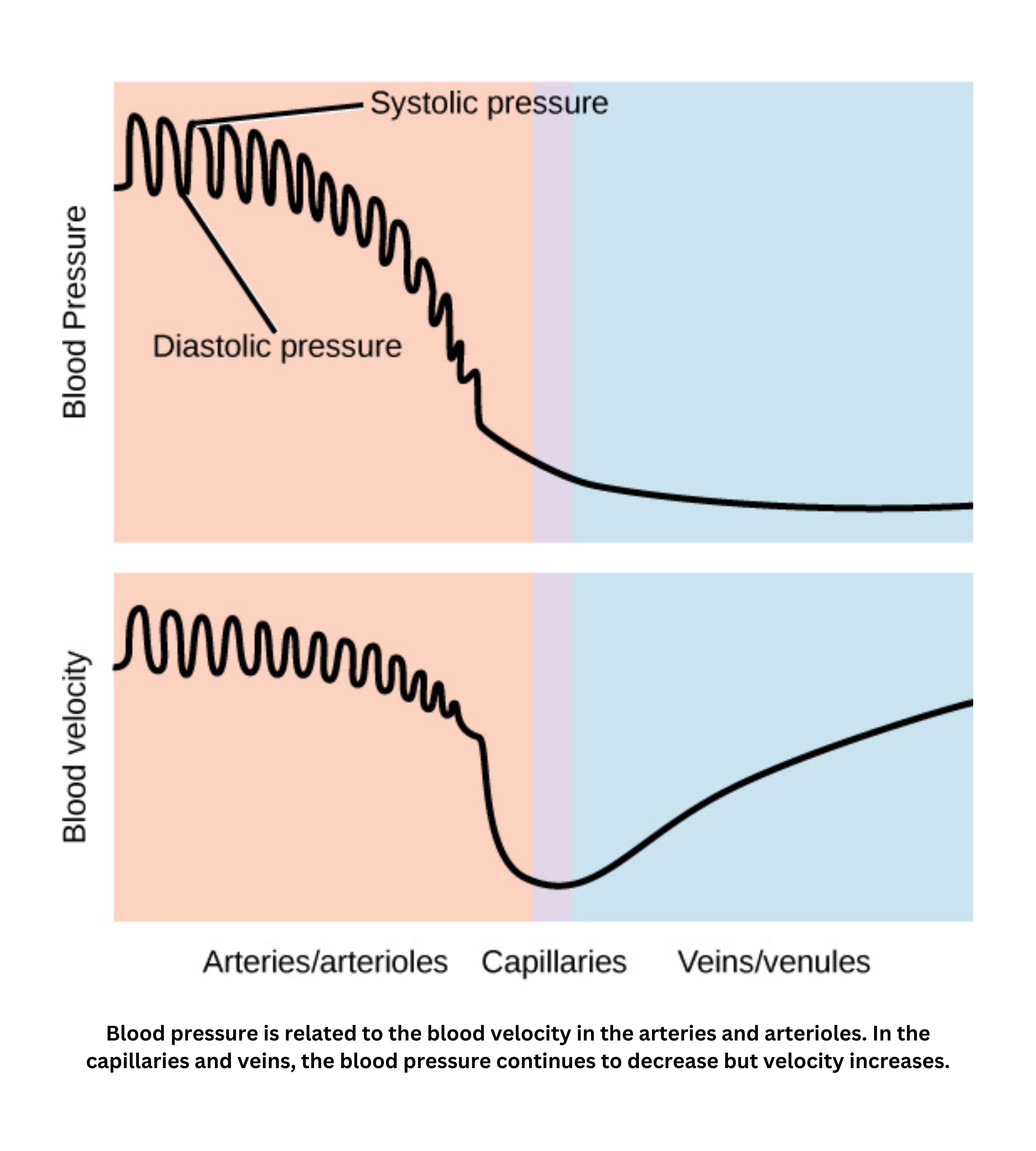
Systolic and diastolic pressure
During a heartbeat:
- Systolic pressure is the pressure in blood vessels when the ventricles contract.
- Diastolic pressure is the pressure when the ventricles relax.
Together, these pressures drive blood through the heart’s chambers, valves, and connecting vessels, sustaining oxygen and nutrient delivery throughout the body.
Pulmonary and systemic circulation
Pulmonary circulation carries deoxygenated blood from the heart to the lungs, where the alveoli reoxygenate it, and then returns oxygenated blood to the heart. Because this circuit is shorter than systemic circulation, it has lower resistance and lower blood pressure.
A key difference in oxygen responses is where vasoconstriction happens:
- In the lungs, low oxygen levels trigger vasoconstriction, redirecting blood toward better-ventilated areas for more efficient gas exchange.
- In the body, low oxygen levels in tissues trigger vasodilation, increasing blood flow to oxygen-starved regions.
Once blood leaves the heart, it flows through…
- larger arteries, which branch into…
- smaller arterioles responsible for controlling blood flow via vasoconstriction and vasodilation. These arterioles lead to…
- capillaries - single-layer endothelium vessels specialized for nutrient and gas exchange.
- Blood then collects in venules and continues into veins on its way back to the heart.
Composition and constriction of blood vessels by type
Arteries, especially elastic arteries like the aorta, have considerable elastic tissue to handle the pressure from each heartbeat.
Muscular arteries distribute blood to specific organs, containing more smooth muscle to regulate vessel diameter.
Capillaries, by contrast, lack smooth muscle and do not actively constrict, focusing instead on gas and solute exchange, while smaller bronchiole-like arterioles are the primary regulators of blood flow through constriction and dilation.
Venule vessels bridge the gap between capillaries and veins, gradually increasing in size but lacking the ability to constrict.
A vein typically features endothelium, smooth muscle, and connective tissue, returning blood to the heart at relatively low pressure. Valves in veins prevent backflow, and adaptations like the respiratory pump (changes in chest and abdominal pressure) and muscular pump (skeletal muscle contractions) aid venous return. Although often thinner-walled than arteries, veins can still constrict via their smooth muscle when stimulated.
Blood pressure and diffusion
Pressure in the circulation is highest in arteries (especially the aorta) and steadily decreases through arterioles, capillaries, venules, and finally the veins (lowest in the vena cava). Elastic recoil in arteries helps maintain forward blood flow during diastole, preventing pressure from dropping to zero.
Within capillary beds, a single cell layer of endothelium allows efficient diffusion of gases and solutes. Depending on tissue requirements, capillaries can be continuous, fenestrated (with small pores), or sinusoidal (with large pores).
Diffusion occurs readily across thin-walled capillaries, supporting nutrient delivery and waste removal. Thermoregulation in these networks involves heat loss by radiation, conduction, or evaporative cooling, supported by mechanisms such as vasodilation near the skin’s surface.
Blood pressure is regulated by changes in vessel diameter (vasoconstriction or vasodilation) and by hormone levels (e.g., ADH, aldosterone, renin, adrenaline), which modify flow resistance. Factors contributing to peripheral resistance include blood viscosity, total vessel length, and lumen diameter; increased body mass or plaques within vessels can further raise resistance. This interaction between vessel structure, fluid dynamics, and external influences helps maintain adequate circulation and homeostasis.
Composition of blood
Composition of blood includes:
- a liquid component called plasma, composed primarily of water, plasma proteins, electrolytes, gases, nutrients, wastes, and hormones.
- The cellular portion features erythrocytes, known as red blood cells (RBCs), which contain hemoglobin for oxygen and carbon dioxide transport, white blood cells (WBCs or leukocytes) that defend against pathogens, and thrombocytes, known as platelets, which are cell fragments essential for coagulation.
Production and regulation of blood components
In coagulation, the process by which blood transforms from a liquid into a gel-like clot, the liver produces clotting factors like fibrinogen. A cascade of reactions converts fibrinogen into fibrin, which forms a protective mesh over wounds. Platelets initiate this process by aggregating at a wound site and releasing enzymes and chemicals that activate clotting factors. Finally, the clot retracts and compacts, and after the blood vessel is repaired, it dissolves.
New erythrocytes are produced in the bone marrow, while the spleen removes aged and damaged ones, recycling iron and converting heme into bilirubin.
Blood osmolarity affects fluid movement: higher osmolarity pulls water into the bloodstream, whereas lower osmolarity draws it into tissues.
Hormones such as ADH (vasopressin) and aldosterone increase water and salt reabsorption in the kidneys, boosting blood volume. Blood volume is primarily managed by the kidneys regulating the loss of water and sodium in the urine.
The percentage of erythrocytes in blood, known as the hematocrit, is usually around 45%. Oxygen transport depends on hemoglobin’s affinity, which can be altered by factors like pH, temperature, and carbon dioxide levels.
Lastly, myoglobin binds oxygen more tightly than hemoglobin, allowing certain tissues to store extra oxygen for later use.
Nervous and endocrine control in blood pressure and transport
The nervous system and endocrine system work together to regulate blood transport throughout the body.
- The nervous system rapidly adjusts heart rate and modulates vasoconstriction and vasodilation through autonomic signals, allowing quick responses to changes in activity or stress.
- The endocrine system releases hormones - such as adrenaline and norepinephrine - that fine-tune these changes, helping increase blood pressure and promote vasoconstriction during acute stress.
Over longer time scales, systems like the renin-angiotensin-aldosterone system and ADH help regulate blood volume and maintain stable blood pressure by controlling water and salt balance.
Baroreceptors monitor pressure changes and send feedback to both systems, helping ensure tissues receive adequate blood flow under varying conditions.