Lymphatic and immune systems
Lymphatic system
The lymphatic system has several crucial roles:
- Equalization of fluid distribution
- Transport of proteins and large glycerides
- Production of lymphocytes for immune defense
- The return of materials to the blood
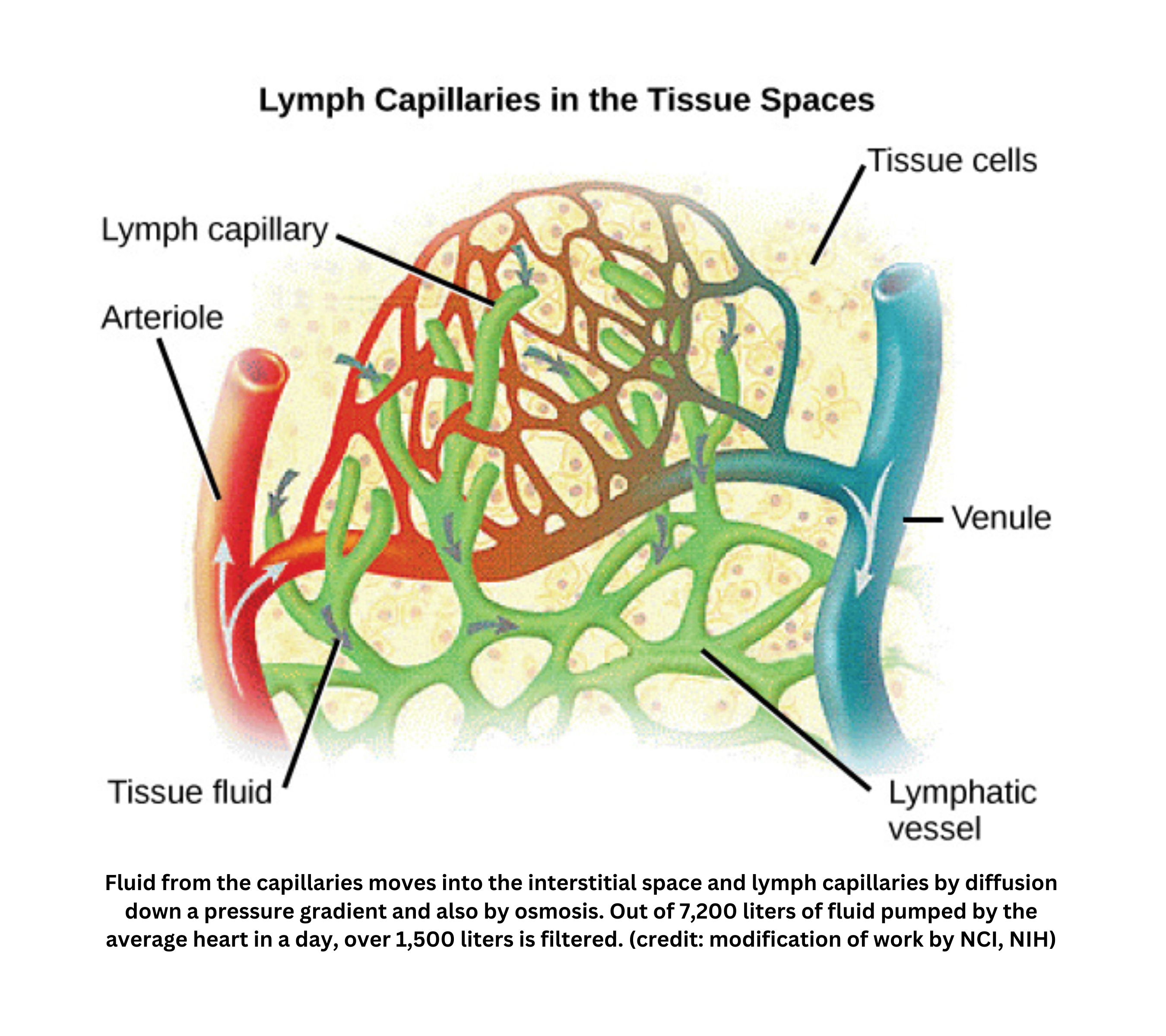
It accomplishes these functions using one-way lymphatic capillaries. These capillaries have flap-like openings that:
- Open when pressure in the surrounding tissue is higher than pressure inside the vessel, allowing interstitial fluid to enter
- Close when the pressure reverses, which prevents backflow
One specialized form of these capillaries, the lacteal, absorbs dietary fats in the small intestine. This helps ensure that large lipids enter lymphatic circulation rather than moving directly into the bloodstream. The system also returns plasma protein that leaks out of blood capillaries, helping maintain proper osmotic balance.
Although lymphocytes originate in the bone marrow, lymphoid tissues such as the thymus (where T cells mature) and clusters of lymph nodes are where these cells reside, proliferate, and differentiate. As white blood cells within lymph nodes filter pathogens and debris, they can become activated and launch an immune response, including antibody production, to protect the body.
Composed mainly of water, proteins, and immune cells, lymph closely resembles blood plasma. It forms when fluid leaves blood capillaries, becomes interstitial fluid, and then diffuses into lymphatic vessels.
Eventually, lymph merges with the veins, returning fluid and proteins to the bloodstream. As lymph passes through lymph nodes, it is filtered. If foreign antigens are detected, resident lymphocytes are triggered to divide and produce defensive molecules. This means leaked fluid, cells, and proteins are not only recovered, but also screened for potential threats before returning to circulation.
Immune system
Innate (non-specific) vs. adaptive (specific) immunity
- The immune system defends the body through both innate immunity and adaptive immunity. Innate immunity provides a rapid, general response to anything foreign, while adaptive immunity mounts a highly specific defense against particular pathogens or antigens.
Several types of white blood cells coordinate these responses:
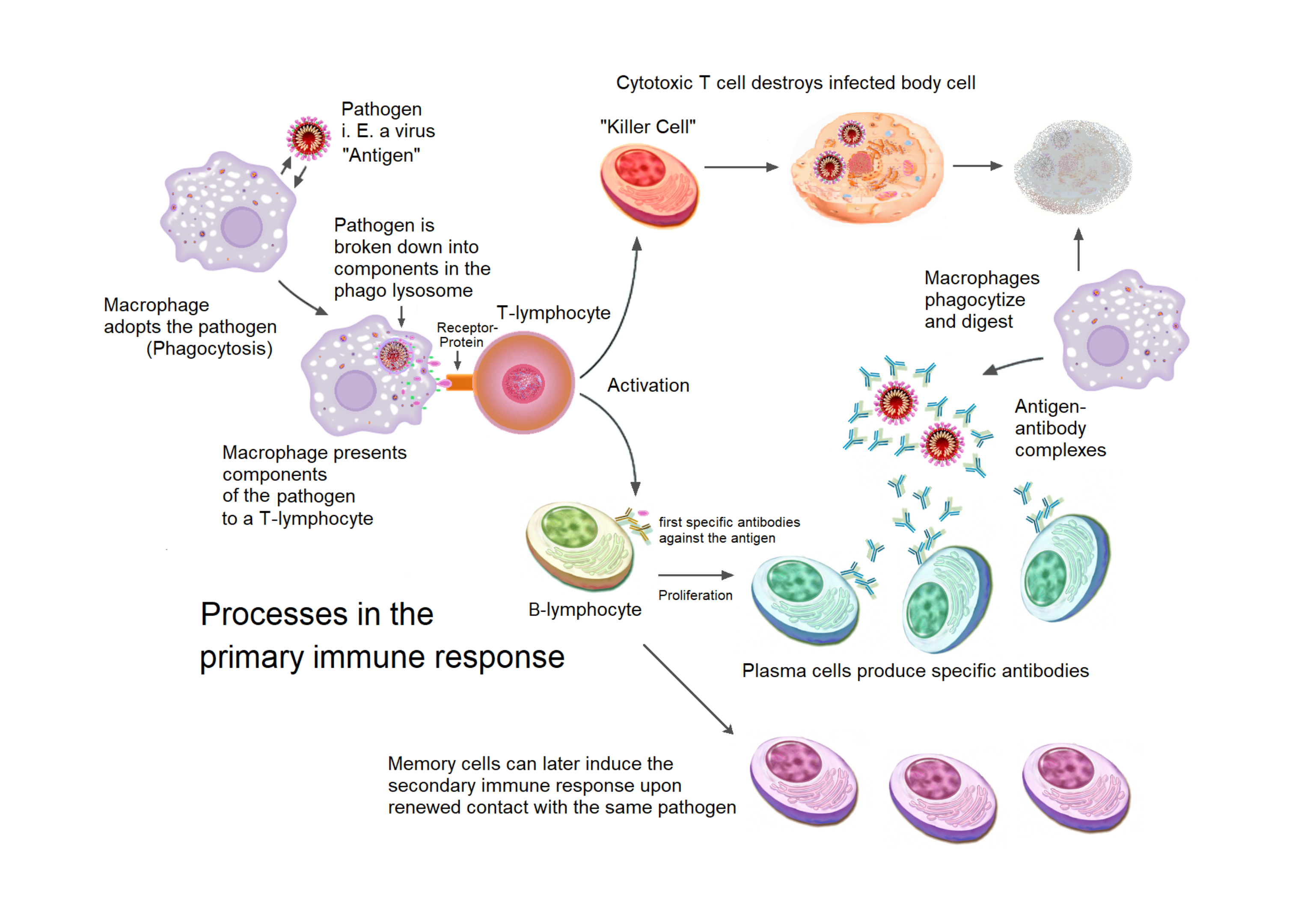
- Macrophages engulf microbes and present portions of their antigens to other immune cells, linking innate and adaptive systems.
- Neutrophils are fast responders that ingest and destroy pathogens.
- Mast cells release histamine during allergic reactions, increasing inflammation.
- Natural killer cells target infected or abnormal cells and induce their destruction.
- Dendritic cells excel at capturing pathogens and displaying their antigens to activate T cells.
- Lymphocytes
- Among lymphocytes, T-lymphocytes mature in the thymus. They include cytotoxic T cells, which trigger apoptosis in infected cells, and helper T cells, which stimulate macrophages, T cells, and B cells.
- B-lymphocytes mature in the bone marrow. After encountering a pathogen, they can differentiate into plasma cells that secrete antibodies or into memory cells that enable a faster response if the same pathogen reappears.
Immune tissues
Immune tissues support these varieties of white blood cells:
- The spleen filters pathogens and old blood cells from circulation.
- Lymph nodes remove pathogens from lymph and house lymphocytes that scan for foreign antigens. When antigens are detected, an immune response initiates, involving inflammation, increased phagocytosis, and, if necessary, production of pathogen-specific antibodies.
- The thymus and bone marrow are also considered immune tissue, as they produce T and B cells.
In innate immunity, physical barriers like skin and mucus membranes help prevent pathogen entry. If pathogens get past these barriers, cells such as phagocytes and natural killer cells, along with antimicrobial proteins, attack invaders non-specifically. The inflammatory response recruits white blood cells to infection sites, and fever can increase immune cell activity.
By contrast, adaptive immunity targets distinct pathogens. Antigen-presenting cells display a pathogen’s foreign markers (antigens) to T and B cells. This can trigger cytotoxic T cells to kill infected cells and helper T cells to activate other immune cells. B cells produce antibodies, Y-shaped proteins that bind antigens for:
- Neutralization
- Opsonization (making pathogens easier for phagocytes to engulf)
- Complement activation (disrupting pathogen membranes)
Over time, memory cells remain and can mount a faster, stronger response upon re-exposure. This helps explain why secondary infections are often milder than the first.
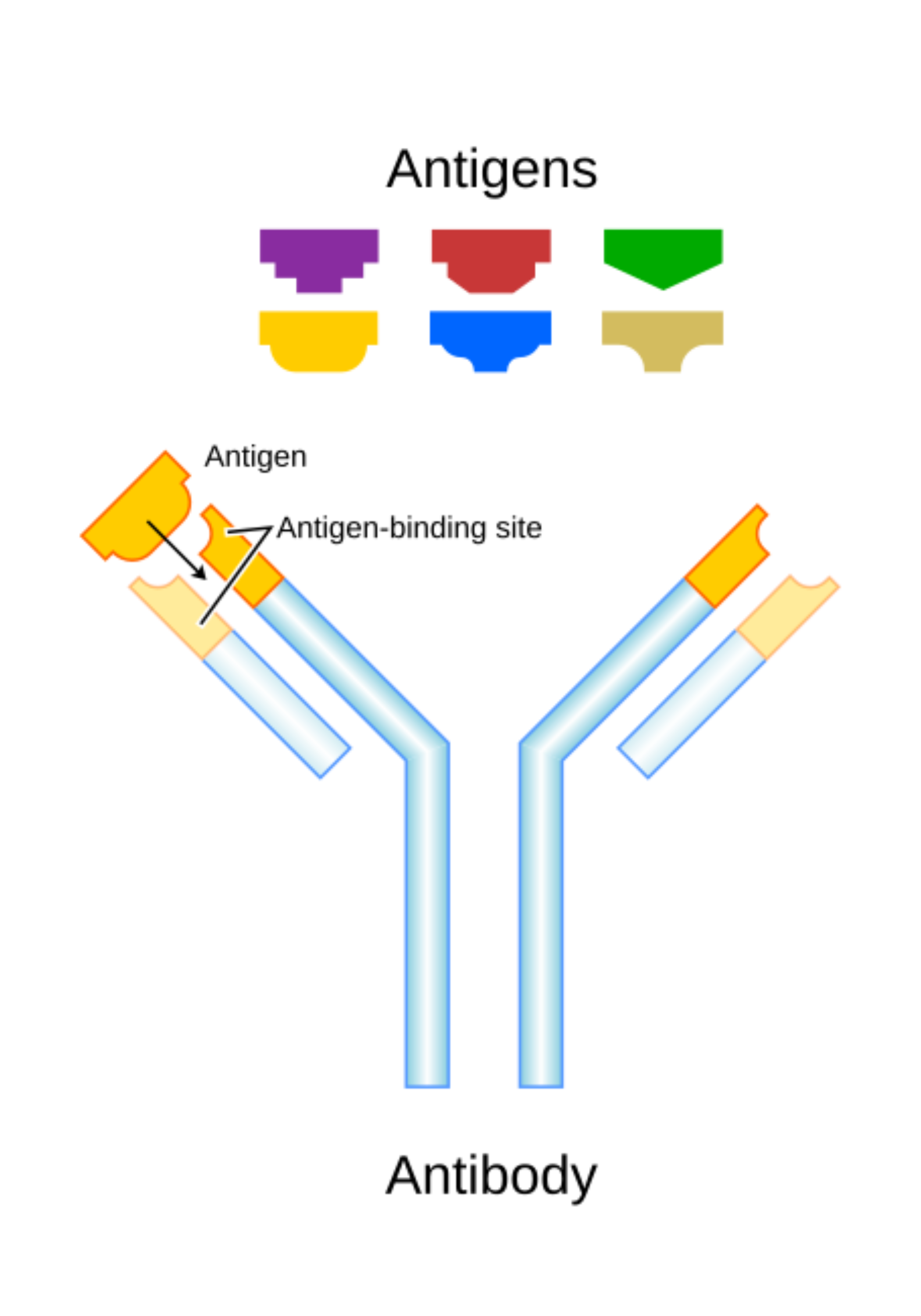
Antigens and antibodies
An antibody contains two light chains and two heavy chains, joined by disulfide bonds. Each tip of the Y shape has a hypervariable region that matches a specific antigen, allowing precise binding.
When a pathogen enters an antigen-presenting cell (APC), it is broken down into fragments, or antigens, and displayed on the cell’s surface. These antigen fragments are recognized by a T cell receptor, triggering immune responses that depend on where the pathogen is located:
- In an extracellular pathogen scenario, a macrophage engulfs the invader and presents the antigen on its surface. A helper T cell recognizes this antigen and signals the macrophage to destroy more of the pathogen, while also activating B cells to produce antibodies.
- If it is an intracellular pathogen, the infected host cell displays antigen fragments on its surface. A cytotoxic T cell detects these fragments and instructs the host cell to self-destruct, eliminating the threat before it can spread.
Clonal selection describes the adaptive immune process in which only the small subset of B or T lymphocytes that recognize a particular antigen multiply into large clones. Once activated by their matching antigen, these lymphocytes proliferate and differentiate into effector cells (such as plasma cells that secrete antibodies) or memory cells that provide long-lasting immunity.
Recognition of self vs. non-self ensures the immune system distinguishes the body’s own tissues from foreign substances. During lymphocyte development, cells that react strongly against the body’s own antigens are usually eliminated or inactivated. When this process fails, autoimmune diseases can arise, with the immune system attacking self-tissues and causing conditions like rheumatoid arthritis or type 1 diabetes.
Finally, the major histocompatibility complex (MHC) is crucial for presenting peptide fragments to T cells. Class I MHC molecules, found on nearly all nucleated cells, present intracellular peptides to cytotoxic T cells, while Class II MHC molecules, restricted to professional antigen-presenting cells (e.g., macrophages, dendritic cells, B cells), display extracellular peptide fragments to helper T cells. This presentation system orchestrates the adaptive immune response by ensuring T cells detect and respond appropriately to foreign antigens.