Muscular and skeletal systems
Muscle system
The muscular system is essential for support and mobility. It generates the force needed to maintain posture, move the body (locomotion), and produce precise movements.
It also contributes to peripheral circulatory assistance by helping move blood and lymph through vessels. When skeletal muscles contract around the deep veins, they compress the veins and help push blood forward. In the cardiopulmonary system, the heart is a muscular pump that circulates blood. The diaphragm also supports circulation: when it contracts during breathing, it helps draw blood into the chest cavity and compresses the abdominal veins.
The muscular system also supports thermoregulation through the shivering reflex. During shivering, rapid, small contractions generate heat.
Structure of muscle types
The muscular system includes three major types of muscle:
- Smooth muscle is nonstriated and involuntary. It’s made of spindle‐shaped cells, each with a single nucleus. It contracts slowly and can sustain prolonged activity without tiring quickly.
- Cardiac muscle is striated and involuntary. It has branching fibers that usually contain one nucleus per cell.
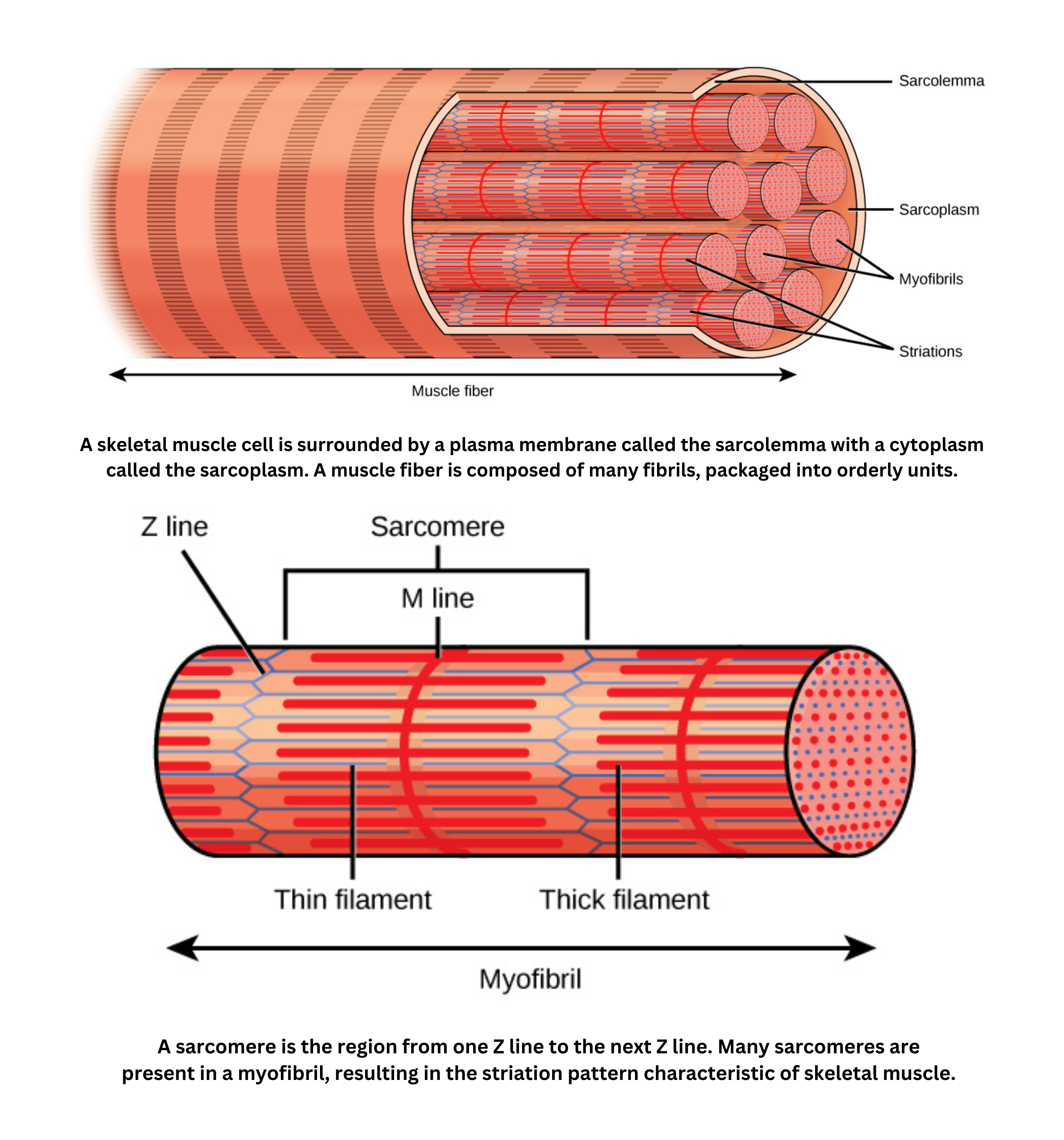
- Skeletal muscle is striated and voluntary. It’s composed of long, multinucleated fibers. It can contract rapidly but fatigues more easily.
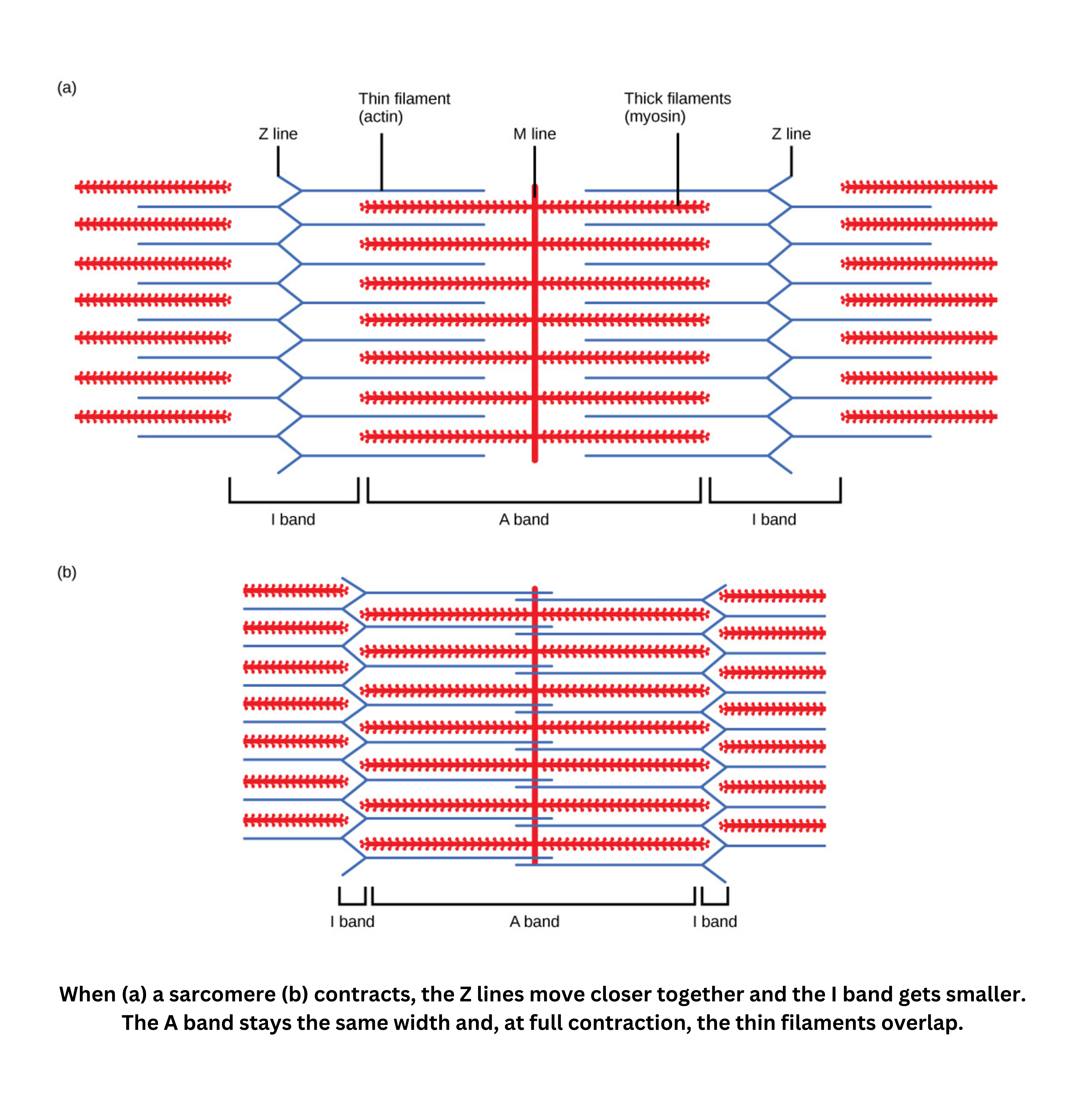
Striations come from repeating units called sarcomeres. The arrangement of actin and myosin filaments in sarcomeres creates alternating dark (A) and light (I) bands.
Smooth muscle still uses the sliding filament mechanism (myosin pulling on actin), but it lacks organized sarcomeres, which is why it appears nonstriated.
Mechanism of contraction
Muscle contraction begins with an electrical signal and ends with force production.
During contraction, the T-tubule system carries electrical impulses deep into the muscle fiber. This signal triggers the sarcoplasmic reticulum to release calcium ions. Calcium then interacts with the contractile apparatus, which is made primarily of actin and myosin filaments. The filaments slide past one another, producing force.
Skeletal muscle contains different fiber types, which affect contraction speed and fatigue resistance. Some fibers contract quickly and generate high force but tire rapidly, while others contract more slowly but sustain activity longer. Because of this, contractile velocity varies across muscle types:
- Fast-twitch (quick bursts)
- Slow-twitch (endurance-focused)
- Smooth muscle contracting more slowly
- Cardiac muscle maintaining a rhythmic, fast-enough pace to circulate blood efficiently.
Force is generated through crossbridges, which form when myosin heads bind to actin filaments and cycle through repeated interactions.
The basic unit of contraction is the sarcomere. A sarcomere is bounded by Z lines, has an M line at its center, and includes an H zone where only myosin filaments are present because actin does not overlap there.
Regulation and fatigue
Troponin and tropomyosin regulate whether myosin can bind to actin:
- When the muscle is relaxed, tropomyosin blocks the myosin-binding sites on actin.
- When calcium binds to troponin, troponin shifts tropomyosin out of the way, exposing the binding sites.
This is why calcium regulation of contraction is central: calcium released from the sarcoplasmic reticulum binds to troponin, which starts the crossbridge cycle and leads to contraction.
Motor neurons control muscle contraction.
- Somatic motor neurons innervate skeletal muscles under conscious control.
- Autonomic motor neurons regulate smooth and cardiac muscle involuntarily.
At the neuromuscular junction, the neuron’s axon terminal releases neurotransmitters onto the motor end plate of the muscle fiber. This triggers an action potential in the muscle fiber, which then leads to contraction.
Voluntary muscles (such as those in the arms and legs) can be activated consciously. Involuntary muscles (such as intestinal smooth muscle and the heart) are regulated by sympathetic and parasympathetic signals, supporting fight‐or‐flight and rest‐and‐digest responses, respectively.
Oxygen debt occurs when muscles rely on anaerobic metabolism during intense exercise because oxygen delivery can’t meet demand. This leads to the buildup of metabolic byproducts and contributes to fatigue.
Skeletal system
The skeletal system provides structural rigidity and serves as the body’s framework. It also stores calcium and can release it under the influence of parathyroid hormones when blood calcium levels drop. Bones protect sensitive organs (for example, the skull protects the brain) and house marrow, where blood cells are formed.
The skeleton includes specialized bone types that match different functions, from load-bearing to fine movement. Joints also vary in structure, from immobile sutures in the skull to freely moving hinge and ball-and-socket joints. Each joint design balances mobility with stability. Humans have an endoskeleton, an internal framework that supports muscle attachment; an exoskeleton encloses the body externally (as in insects).
Bone composition
At the macroscopic level, a bone is a solid structure with internal canals for blood vessels and nerves, along with small cavities where cells reside. Bone tissue is built on a calcium/protein matrix made primarily of calcium salts, collagen fibers, and mineral deposits (largely hydroxyapatite). Together, these components provide tensile and compressive strength.
The cellular composition of bone involves:
- Osteoblasts (forming new bone)
- Osteocytes (maintaining bone tissue)
- Osteoclasts (breaking down bone)
Bone is covered by a membrane rich in stem cells that can give rise to osteoblasts and osteoclasts. Microscopically, bone consists of cells (primarily osteocytes) embedded in an extracellular matrix organized into cylindrical units called osteons, each with a central canal. The matrix is a calcium-protein matrix composed of calcium salts, collagen fibers, and a ground substance that acts like a glue.
Bone growth and remodeling
Bone growth and remodeling depend on coordinated activity between bone-forming and bone-resorbing cells.
- Lengthwise growth happens when osteoblasts add new bone tissue at the knobs (epiphyseal regions) at the ends of long bones. At the same time, osteoclasts resorb and reshape bone tissue to maintain proper size and form.
- Growth in diameter occurs when osteoblasts deposit new bone on the outer surface, while osteoclasts remove bone from the inner surface. This creates a hollow structure, keeping bones strong without making them excessively heavy.
Cartilage, ligaments and tendons
Cartilage provides a flexible cushion at many joints and helps shape structures like the nose and ears. Although it has no direct blood supply, it resists friction and absorbs shock efficiently.
Both ligaments and tendons support skeletal function:
- Ligaments connect bones to one another, stabilizing joints.
- Tendons connect muscles to bone, transmitting force to produce movement.
Endocrine control of the skeletal system relies on hormones such as parathyroid hormone, calcitonin, and vitamin D to regulate bone remodeling and calcium homeostasis, supporting strong bones and balanced mineral levels.
Specialization of bone types
The skeletal system includes specialized bone types and joints that work together to provide support and mobility. Long bones are rod-shaped and form the arms, legs, and fingers, providing leverage and support for movement. Short bones are roughly cube-shaped and are found in the wrist and ankle, where stability is prioritized over extensive movement. Flat bones are thin and broad - such as those in the sternum, scapulae, ribs, and skull - supporting protection and providing broad surfaces for muscle attachment. Irregular bones have complex shapes, such as vertebrae and hip bones, and don’t fit neatly into the other categories.
Joint structures
A joint is the location where two bones meet, and joints can be mobile or immobile.
Mobile joints (synovial joints) contain a fluid-filled cavity that lubricates and supports movement. Examples include:
- the ball-and-socket joint (shoulder and hip), which allows the greatest range of motion
- the hinge joint (such as the elbow), which permits bending and straightening
- the gliding joint (as in the wrist), which enables sliding movements.
Non-mobile joints connect bones with cartilage or fibrous tissue. Examples include the sutures in the skull and the rib-to-sternum connections, which provide stability with little or no movement.
Endoskeleton vs. exoskeleton
Humans have an endoskeleton, an internal framework that supports the body. An exoskeleton is an external structure made of chitin, as seen in insects.