Prescription intake and order entry
Most prescriptions are paper prescriptions (also called written prescriptions). Traditionally, paper prescriptions are handwritten and signed by the prescriber. A paper prescription may also be computer-printed and then manually signed by the prescriber.
Some prescriptions are telephonic (verbal), where the prescriber or an authorized agent calls the prescription in to the pharmacy. Prescriptions can also be transmitted as facsimiles (faxed). Many prescribers are increasingly using e-prescriptions; sending a prescription electronically is called e-prescribing.
In inter-pharmacy transfers, prescriptions are transferred electronically between two pharmacies.
Prescription intake
Prescription intake is one of the pharmacy technician’s responsibilities. When the pharmacy receives a prescription, it’s tracked using prescription origin codes (POC). The prescription origin codes are as follows:
Pharmacy prescription origin codes (POC)
| POC | Meaning |
|---|---|
| 0 | Unknown: This is used when the method of receiving the original prescription is unknown, which may be the case in a transferred prescription. |
| 1 | Written prescription via paper, which includes computer-printed prescriptions that a physician signs as well as traditional prescription forms |
| 2 | Telephonic prescription |
| 3 | E-prescriptions |
| 4 | Facsimile prescription obtained via fax transmission |
All prescriptions must be checked for accuracy and completeness. Tamper-resistant prescription forms are required when prescribing controlled substances.
Parts of a prescription are as follows:
- Patient identifiers: This includes the patient’s full name, physical address, and date of birth.
- Prescriber identifiers: The full name, title (e.g., MD, DO), physical address of the practice, and telephone number.
- Date when the prescription was issued.
- Medication details: Drug name, strength, Sig code indicating details such as how many tablets and how frequently to take the drug, quantity to dispense, the diagnosis code (as per ICD), days’ supply, and number of refills.
- DEA and NPI number: All prescribers need a DEA number to prescribe controlled substances. This allows the DEA (Drug Enforcement Administration) to track the use of controlled substances. Each DEA number is a combination of 7 numbers and 2 letters. The first letter is the prescriber code that identifies the type of prescriber (hospital, clinic, etc.), while the second letter stands for the first letter of the prescriber’s last name. The second letter is replaced by the number “9” in the case of a business name instead of a provider name. Examples of DEA numbers include FD3456781, F93456781. The NPI (National Provider Identifier) number is a 10-digit unique number essential to order or write prescriptions. It is also required to process health insurance claims and authorizations.
- Prescriber signature.
DAW codes
“Dispense As Written” (DAW) codes, also called product selection codes, indicate what type of product is allowed: brand name or generic substitution. The DAW code is found on the prescription.
| DAW code | Meaning |
|---|---|
| 0 | No product selection indicated; default |
| 1 | Substitution not allowed by prescriber |
| 2 | Substitution allowed - patient-requested product dispensed; used when a patient requests a specific brand of drug |
| 3 | Substitution allowed - pharmacist selected product dispensed; used when the pharmacist determines that the brand product should be dispensed. |
| 4 | Substitution allowed - generic drug not in stock when the pharmacist dispenses brand name drug due to lack of availability of generic drug. |
| 5 | Substitution allowed - brand drug dispensed as generic |
Data from the prescription is recorded in the pharmacy database. In addition to the details on the prescription, the pharmacy may also record:
- Drug allergies
- The patient’s contact number
- Current insurance information
- The planned pickup time (community pharmacy)
Controlled substances also require government-issued ID verification.
How to calculate days’ supply: Days’ supply is an estimate of how many days a prescription is intended to last. It’s computed by dividing the number of doses in the prescription by the number of doses per day.
Calculating days’ supply depends on the dosage form (tablets, suspensions, injectables, etc.).
Calculating days’ supply for tablets and capsules: For example, the prescription states, "Tablet Amoxicillin 500 mg tid for 7 days
21 tablets". The days’ supply is calculated as follows:
Days’ supply = Number of doses in the prescription / Number of doses per day = 21/3 = 7 days supply
Calculating days’ supply for liquids: For example, if the prescription states, “Amoxicillin 400 mg/5ml 200 ml, 2 tsp q12h x 10 days”, it means a total of 200 ml has to be dispensed. Convert teaspoons to ml: 1 tsp = 5 ml, so each dose is 10 ml and the daily dose is 20 ml.
Days’ supply = 200 ml/20 ml = 10 days’ supply.
PRN dosing: When the prescriber states that a medication can be used “as needed” or “prn,” calculate using the highest dose and the shortest interval.
For example, the prescription states, " Tablet Ibuprofen 400 mg #30 1-2 tabs po q6-8h prn for pain." The highest dose is 2 tablets, and the shortest interval is every 6 hours. Decimals have to be rounded off.
Days’ supply = 30/2x4 = 30/8 = 3.75, about 4 days’ supply.
Calculating days’ supply for ointments and creams: For creams and ointments, a single dose ranges from 0.5-1 gram. The dose also varies depending on the size of the affected area. Sometimes, prescriptions may mention doses in finger-tip units. 1 finger-tip unit (FTU) equals 0.5 gram. 1 FTU can be applied over an area that corresponds to double the size of the flat of a hand.
For example, the prescription states, “Desonide 0.05% ointment, apply thin film tid, dispense 30 g.”
In this case, 0.5 g is a better dose indicator because the instruction is to apply a thin film.
Days’ supply = 30 g/1.5 g = 20.
Calculating days’ supply for inhalers and sprays: The package of inhalers and sprays lists the total number of inhalations, actuations, or metered doses per container. Each dose is typically 1-2 puffs or sprays and is stated on the prescription.
For example, the prescription states, “Advair 125-25 MCG inhaler, 2 sprays qd x 1 month,” and the package states 60 metered actuations.
Days’ supply = 60/2 = 30.
Calculating days’ supply for Insulin: Insulin is packaged in vials, pens, syringes, and pumps. Insulin dosing is stated as the number of “Units” of insulin. Standard insulin contains 100 units in 1 mL (U-100 insulin). Insulin syringes are marked as 1-2 units per small marking depending on the syringe size (e.g., 50 U versus 100 U syringe). More concentrated insulins, such as U-300 and U-500, have recently become available.
Each insulin package may have a single multidose vial or multiple vials or pens. To calculate the days’ supply, first calculate the total number of insulin units in the package.
For example, 1 package of Humalog carries one 10 ml vial of strength 100 U/ml. Hence, 1 package has a total of 10 x 100 = 1000 Units of insulin. Similarly, one package of Humulin N Kwikpen has five 3 ml pens of strength 100 U/ml. Hence, the total dose per package is 100 x 3 x 5 = 1500 units.
Dividing the total units in the package by the number of units taken each day gives the days’ supply of insulin. The days’ supply must never exceed the expiration date after opening. If the days’ supply calculation yields a decimal number, then drop the decimal (e.g., convert 25.45 to 25).
For example, a prescription for Humulin U-100 states, " Administer 50 U subcutaneously 30 mins before breakfast and dinner." Considering it has a single 10 ml vial containing 100 U/ml, the total dose in the package is 1000 units.
Days’ supply = 1000 / 50+50 = 1000/100 = 10 days’.
Calculating days’ supply for injectables: This is similar to insulin, except that instead of Units, use milliliters (ml). Divide the total number of milliliters available (in vials, ampules, or syringes) by the number of milliliters used per day.
For example, if the prescription for a 5 ml package of injection triamcinolone 40 mg/ml states, “Inject 20 mg im q12h.” The total daily dose is 40 mg, which equals 1 ml/day.
Daily dose = 5 ml/1 ml = 5 days.
Calculating the days’ supply for eye and ear drops: A standard dropper delivers about 20 drops/ml (20 gtt/ml). Days’ supply is calculated by dividing the total number of drops dispensed by the number of drops required per day.
For example, the Sig code for Latanoprost eye drop 0.005% dispensed as a 2.5 ml bottle states “1 gtt ou bid”.
2.5 ml = 2.5 x 20 = 50 drops total
Daily dose = 4 drops per day (includes both eyes)
Days’ supply = total number of drops dispensed / daily dose in drops = 50/4 =12.5 days
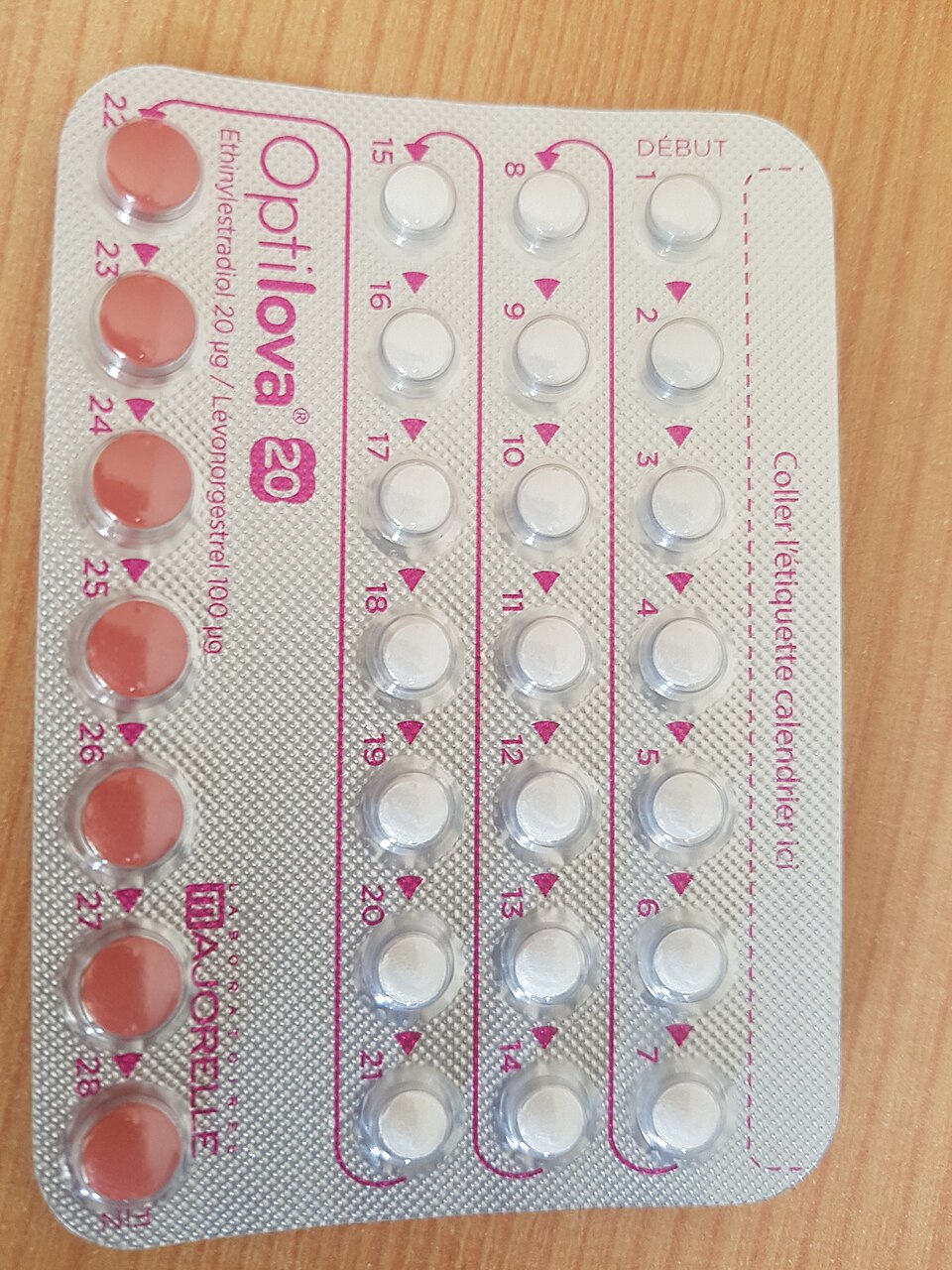
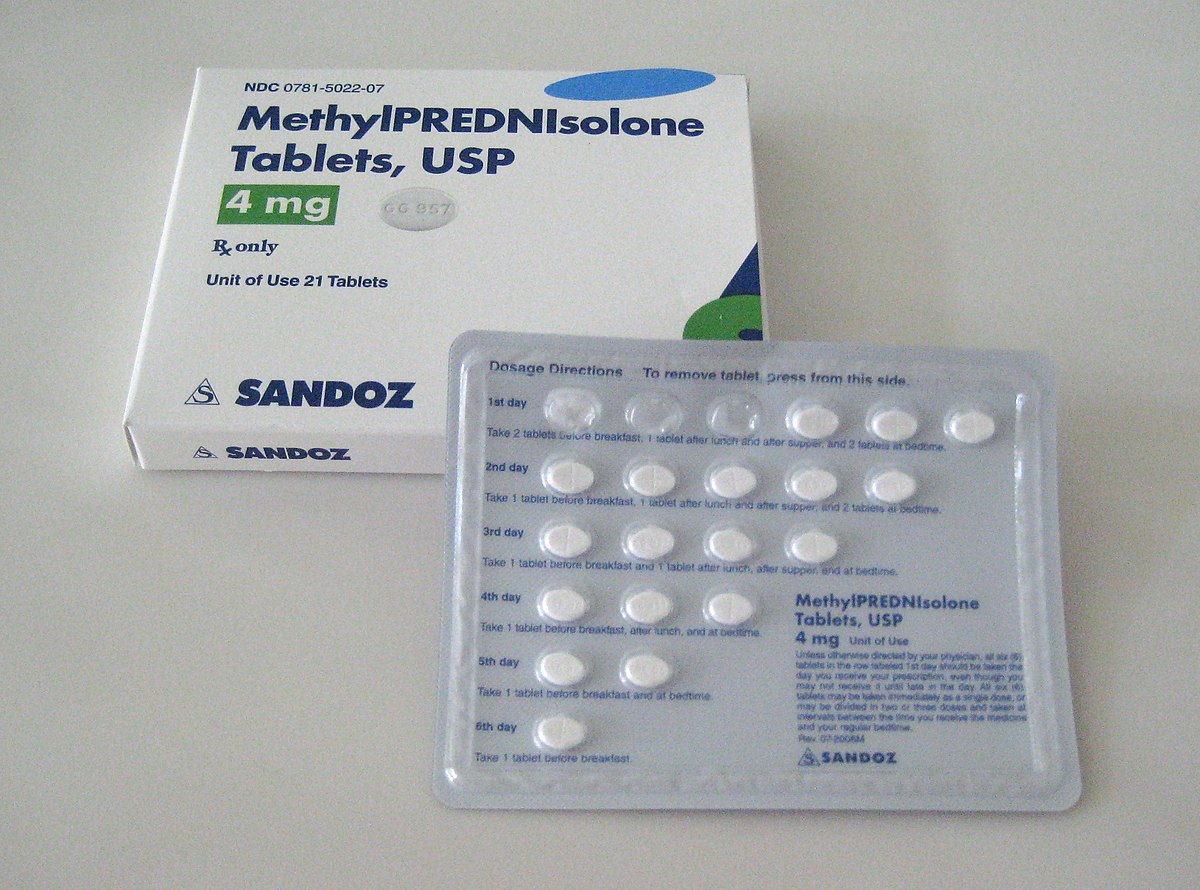
Days’ supply for packs: Certain medications (such as birth control pills, steroid tablets, and certain antibiotics like Azithromycin) are dispensed as readymade packets. Each packet includes instructions that indicate the days’ supply.
For example, a Z pack for Azithromycin states how many tablets to take on days 1 to 5, so the days’ supply is 5 days. Similarly, birth control pills come in 21-day or 28-day packets, so the days’ supply is 21 or 28 days per packet, respectively.
Refills: The number of refills is written on the prescription. Even when a prescription is written for a 90-day (3-month) supply, insurance may only allow a 30-day fill at one time. This also depends on the medication type. If a refill is requested too early, insurance will reject it.
In special circumstances (such as traveling abroad), an early refill may be requested. Many insurance plans require prior approval for early refills. A new prescription is required if the prescription is over a year old.
A partial fill is done when the pharmacy doesn’t have enough stock to fill a prescription or refill. A 2-5 day supply of medication can be dispensed until the pharmacy can fill the balance of the prescription.
State and federal laws dictate how controlled substances are refilled:
- Schedule II medications cannot be refilled. A new prescription is required for every fill.
- Generally, the prescription has a validity of six months.
- Schedule III and IV medications cannot be refilled after six months or five times, whichever is earlier.
- Generally, prescribers write sequential prescriptions for Schedule II medications, with a “Do not fill until” date on each prescription.
- Schedule V medications may be written for up to 1 year, although many states limit this to 6 months.
Legend medications: A legend drug is a medication that requires a prescription. A legend drug can be dispensed upon receipt of a prescription from a licensed healthcare provider. It is labeled with the legend “Rx” only. OTC (over-the-counter) medications are also known as “non-legend” medications because they do not require a prescription.
Order entry
Once the prescription is received, the order must be entered into the pharmacy management system. Details from the prescription (as discussed above in prescription intake) are entered into the system along with a copy of the prescription itself.
At this stage, the pharmacy also typically:
- Schedules a pickup time or delivery services
- Updates allergy and contact information
- Checks drug inventory status to avoid delays in filling and processing medications
The correct NDC number needs to be selected at this stage. NDCs change with manufacturers, dosage forms, strengths, and packaging. So even the same active ingredient, such as Prednisone, will have multiple NDC numbers.
Pharmacy benefit managers (PBM) serve as intermediaries between the pharmacy, drug manufacturers, and insurance companies. They are closely associated with formulary design, utilization management, price negotiation, pharmacy network formation, and mail-order pharmacy services. The three largest PBMs are Express Scripts, OptumRx, and CVS Caremark.