Lymphedema
Anatomy and physiology
Lymphatic physiology
- Works simultaneously with the venous system for fluid return
- Removes plasma proteins
- Filters antigens, bacteria, and waste products
- Produces white blood cells, specifically lymphocytes
- All white blood cells originate in the bone marrow; organs within the lymphatic system, like the thymus, spleen, and lymph nodes, are crucial for their development and function.
Lymph nodes
A series of sinuses that filter antigens and bacteria. The plasma that seeps out of blood capillaries into the surrounding tissues forms lymph fluid. * Key to immunological response
- Total in the body = 600, with 300 in the head/neck
Two primary lymphatic ducts of the body
- Right lymphatic duct
- Thoracic duct
Lymph fluid composition
- Transparent, yellowish fluid containing water, proteins, lipids, minerals, and hormones
- The human body produces 2.4 L of lymph fluid daily.
- 25 L cycles through the heart
Pathology
Lymphedema
- Excessive accumulation of lymph fluid due to dysfunction in the lymphatic system, leading to increased edema
- Causes: Surgery, physical trauma, radiation, infection, etc
Effects of lymphedema
- Chronic swelling
- Excessive tissue proteins
- Fibrotic changes
- Chronic inflammation
- Infections – cellulitis
- Skin changes – 'peau d’orange’- a medical term describing a characteristic appearance of the skin (skin of an orange)
Related impairments
- Functional deficits
- Loss of mobility
- Difficulty wearing normal clothing
- Psychological issues
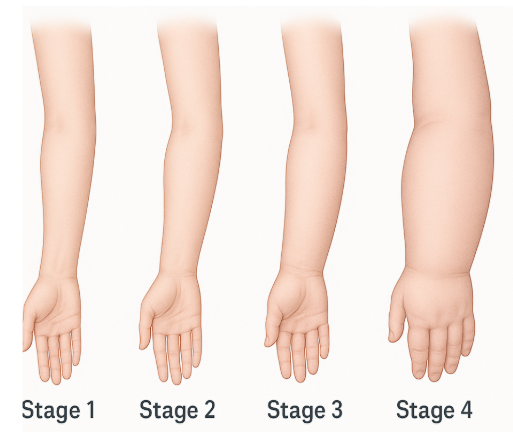
Stages of lymphedema
Stage 1
- Latent, subclinical condition
- Swelling not evident despite impaired lymph system
Stage 2
- Completely and spontaneously reversible
- Soft, pitting edema
- Little to no fibrosis
- Skin easily pinched and moved
- Stemmer sign present
Stage 3
- Spontaneously irreversible
- Tissues are usually fibrotic
- Pitting requires strong pressure or no pitting
- Can usually be reversed with treatment
- Stemmer sign present
Stage 4 — Elephantiasis
- Irreversible
- No pitting, significant fibrosis
- Hardening of the skin
Goals of manual lymph drainage
- Peristalsis of lymph fluid
- Breakdown of fibrotic tissues
- Increase lymph volume in lymph vessels
- Decrease congestion in the interstitium
Basic principles
- Treatment always begins proximally to clear proximal lymph nodes before moving to affected lymphotomes (a specific region of the skin that drains lymph to a particular group of lymph nodes).
- Massage is directed towards the cleared lymph node
- Pressure is very light
Contraindications
- Bacterial infection
- Acute congestive heart failure
- Acute deep vein thrombosis
- Acute renal disease
- Acute pulmonary edema
- Malignancy
- Arterial disease
- Sensation deficits
- Low blood counts
- Areas of inflammation
- Open wounds
Bandaging techniques
Compression garments
- Maintains the reduction gained during therapy
- Transition to garments when reduction plateaus
- Garments for daytime wear, options for nighttime
- Insurance coverage varies greatly
Therapeutic exercise
- Exercises facilitate muscle pumping
- Should be done with compression
- Progress from proximally to distally
- Very low resistance
Patient education
- Home exercise
- Self-massage
- Skin care
- Precautions
- Compression garments