Endocrine and metabolic systems
Endocrine system
Thyroid disorders
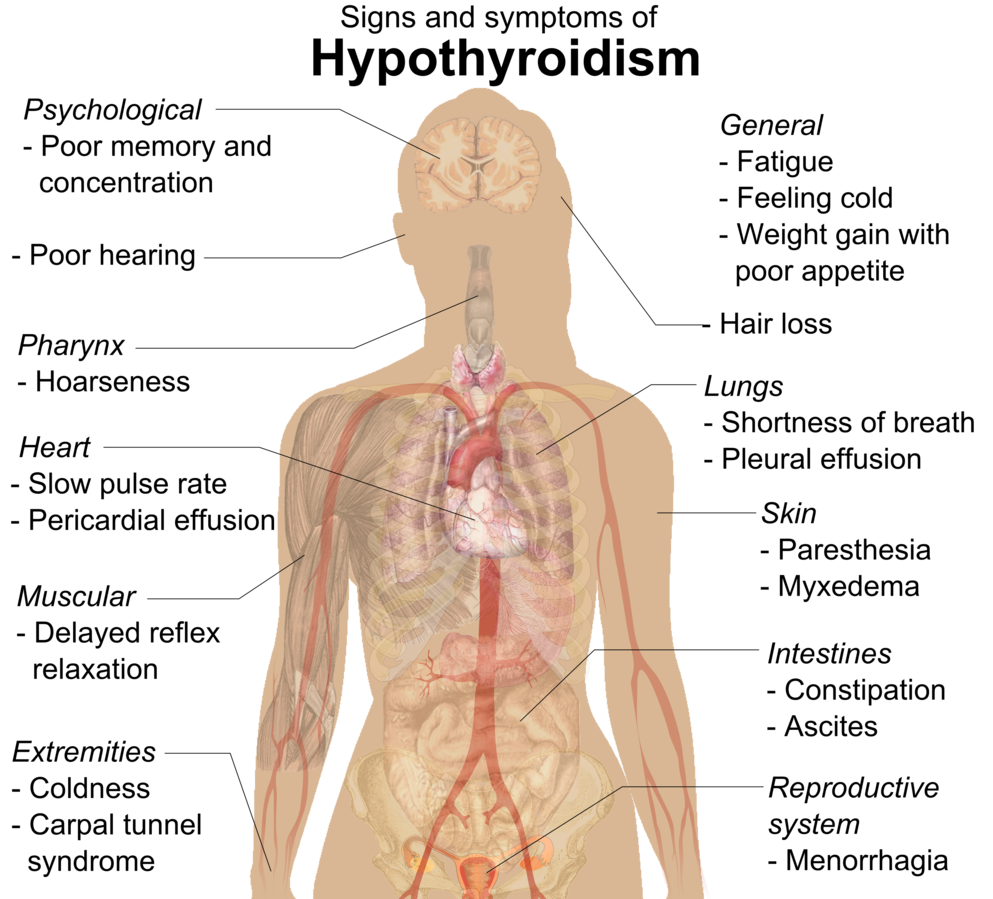
Hypothyroidism (underactive thyroid)
- Cause: Autoimmune disease (Hashimoto’s thyroiditis), iodine deficiency, post-thyroidectomy.
- Symptoms: Fatigue, weight gain, cold intolerance, bradycardia, constipation, depression, myopathy, slow DTRs.
- PT implications:
- Monitor for exercise intolerance, muscle weakness, and risk of rhabdomyolysis.
- Low-intensity exercise with gradual progression.
- Watch for joint stiffness and slowed healing.
Hyperthyroidism (overactive thyroid)
- Cause: Autoimmune disease (Graves’ disease), excess iodine, thyroid tumors.
- Symptoms: Weight loss, heat intolerance, tachycardia, hyperreflexia, muscle wasting, tremors, exophthalmos (bulging eyes).
- PT implications:
- Monitor HR and BP due to risk of tachycardia, arrhythmias, and hypertension.
- Heat intolerance → Adjust the exercise environment.
- Avoid high-intensity exercise due to risk of fatigue and catabolic muscle loss.
Thyroid storm (medical emergency)
- Acute hyperthyroidism crisis with severe tachycardia, fever, and confusion → Requires emergency care.
Adrenal gland disorders
The adrenal glands (on top of the kidneys) produce cortisol, aldosterone, and catecholamines (epinephrine, norepinephrine).
Addison’s disease (adrenal insufficiency)
- Cause: Autoimmune destruction of adrenal glands → Decreased cortisol and aldosterone.
- Symptoms: Fatigue, hypotension, weight loss, salt craving, hyperpigmentation, weakness.
- PT implications:
- Monitor for hypoglycemia, hypotension, and fatigue.
- Avoid overexertion due to limited stress response.
- Risk of adrenal crisis (severe hypotension, dehydration, shock) → Medical emergency!
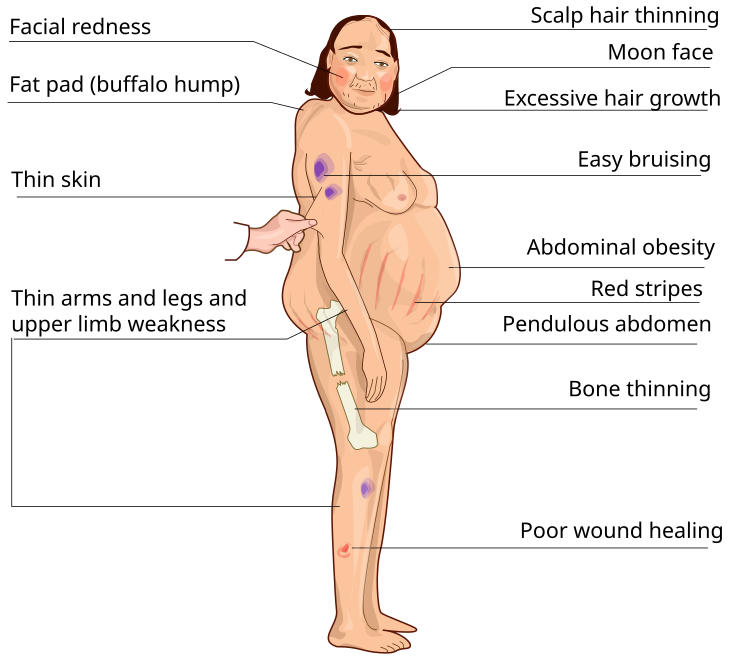
Cushing’s syndrome (hyperfunction of adrenal glands)
- Cause: Excess cortisol from long-term steroid use or an adrenal tumor.
- Symptoms: Moon face, buffalo hump, central obesity, muscle atrophy, osteoporosis, hypertension, poor wound healing.
- PT implications:
- Fall risk due to osteoporosis and muscle weakness.
- Monitor BP and glucose levels (risk of hypertension and diabetes).
- Avoid high-impact exercises to prevent fractures.
Diabetes mellitus (DM)
Type 1 diabetes (insulin-dependent)
- Cause: Autoimmune destruction of pancreatic beta cells → No insulin production.
- Symptoms: Polyuria, polydipsia, polyphagia, weight loss, ketoacidosis (DKA risk).
- PT implications:
- Monitor for hypoglycemia (shakiness, confusion, sweating, dizziness).
- Exercise increases insulin sensitivity → Adjust insulin and carb intake accordingly.
- Avoid exercise during peak insulin activity to prevent hypoglycemia.
Type 2 diabetes (insulin-resistant)
- Cause: Insulin resistance due to obesity, genetics, and a sedentary lifestyle.
- Symptoms: Polyuria, polydipsia, slow wound healing, neuropathy, blurred vision, fatigue.
- PT implications:
- Encourage aerobic and resistance exercise to improve insulin sensitivity.
- Monitor for neuropathy and fall risk.
- Check for foot ulcers and skin integrity.
Associated diabetic conditions
- Hypoglycemia
- Cause: Low blood sugar (<70 mg/dL)
- Symptoms: Sweating, confusion, dizziness, tachycardia
- PT considerations: Provide glucose immediately (juice, glucose tablets)
- Diabetic Ketoacidosis (DKA)
- Cause: No insulin production causes fat breakdown and release of ketones in the bloodstream
- Symptoms: Fruity breath, deep breathing (Kussmaul), nausea, confusion
- PT considerations: Medical emergency! No exercise!
- Peripheral Neuropathy
- Cause: Nerve damage from prolonged hyperglycemia
- Symptoms: Numbness, tingling, burning pain in feet/hands
- PT considerations: Foot care education, balance training, fall prevention
- Diabetic retinopathy
- Cause: Retinal blood vessel damage due to hyperglycemia
- Symptoms: Vision loss, blurred vision
- PT considerations:Avoid head-down exercises, and high-impact exercises that can raise blood pressure increasing pressure on the damaged retinal vessels.
- Nephropathy
- Cause: Kidney damage from diabetes due to hyperglycemia
- Symptoms: Protein in urine, swelling, hypertension
- PT considerations: Monitor hydration levels and blood pressure
- Peripheral Artery Disease (PAD)
- Cause: Poor circulation in legs due to vascular damage from hyperglycemia
- Symptoms: Claudication (leg pain with walking), cold feet
- PT considerations: Use graded walking program
Safe blood sugar levels for physical therapy
Before you begin
- If blood sugar is less than 90 mg/dL: Have a small carbohydrate snack (15-30g) and have patient recheck glucose levels. .
- If blood sugar is 90-124 mg/dL: Proceed with exercise.
- If blood sugar is 126-250 mg/dL: Safe to exercise.
- If blood sugar is over 250 mg/dL: Patient should check for ketones in your urine.
- If ketones are present: Do not exercise, as this can lead to diabetic ketoacidosis.
- If no ketones are present: Exercise cautiously, monitor closely, and stay hydrated.
During and after exercise
- Monitor frequently: Check your blood sugar every 30 minutes during activity, especially if it’s high-intensity or you are a type 1 diabetic on insulin.
- Stay hydrated: Drink plenty of fluids before, during, and after exercise.
- Be prepared: Always carry fast-acting carbohydrates (like fruit or juice) to treat low blood sugar in case it drops unexpectedly.
Metabolic disorders
The metabolic system includes chemical processes that maintain life, including energy production and nutrient utilization.
Osteoporosis
- Cause: Decreased bone density (aging, menopause, steroid use, hyperthyroidism).
- Symptoms: Fractures, kyphosis, back pain.
- PT implications:
- Weight-bearing exercise to improve bone density.
- Avoid spinal flexion exercises to prevent vertebral fractures.
- Balance training to prevent falls.
- DEXA (Dual-Energy X-ray Absorptiometry) scans are used to measure bone mineral density and are the most accurate way to assess bone health.
- Determined by T-score:
- Normal: less than -0.1
- Osteopenia : -1.0-(-2.5)
- Osteoporosis: greater than -2.5
- Determined by T-score:
Paget’s disease
- Cause: Excessive bone turnover → Weak, deformed bones.
- Symptoms: Bone pain, deformities, fractures, and hearing loss.
- PT implications:
- Low-impact exercise to maintain mobility.
- Monitor for fractures and joint dysfunction.
Gout (metabolic arthritis)
- Cause: Uric acid crystal buildup in joints (linked to diet, kidney dysfunction).
- Symptoms: Severe joint pain (big toe common), redness, swelling.
- PT implications:
- Avoid excessive weight-bearing during flares.
- Encourage hydration and dietary modifications (low purine diet)
Metabolic syndrome
Criteria for metabolic syndrome:
- Abdominal obesity
- Waist circumference:
- Men: >40 inches (102 cm)
- Women: >35 inches (88 cm)
- Waist circumference:
- Elevated blood pressure
- ≥130/85 mmHg or taking antihypertensive medication
- Elevated fasting blood glucose
- ≥100 mg/dL or diagnosed diabetes
- High triglycerides
- ≥150 mg/dL or taking medication for high triglycerides
- Low HDL (good cholesterol)
- Men: <40 mg/dL
- Women: <50 mg/dL
Causes and risk factors
- Lifestyle Factors: Poor diet, sedentary lifestyle, obesity
- Genetics: Family history of diabetes or cardiovascular disease
- Hormonal Imbalance: Insulin resistance, PCOS (in women)
Symptoms
- Often asymptomatic until complications arise
- Signs may include increased waist size, fatigue, high blood sugar symptoms (thirst, frequent urination), and high blood pressure
PT considerations
- Exercise recommendations:
- Focus on aerobic exercise (brisk walking, cycling, swimming)
- Include resistance training to improve insulin sensitivity
- Gradual progression to prevent fatigue and improve adherence
- Weight management: Encourage lifestyle changes like a healthy diet and activity
- Blood pressure monitoring: Avoid high-intensity exercises if diabetes is uncontrolled