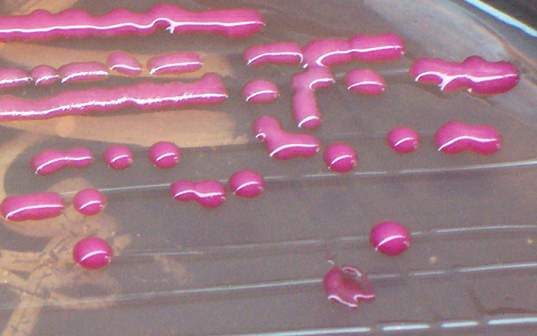Klebsiella pneumoniae
It’s usually considered a nosocomial pathogen and is widely known for antibiotic resistance, including ESBLs (extended-spectrum beta-lactamases).
Human pathology
It’s mainly associated with:
- Respiratory infections such as pneumonia and lung abscess
- UTIs
- Wound infections
- Sepsis
- Meningitis
You’ll most often see it in hospital settings or in immunodeficient individuals, such as older adults, people with chronic diabetes, and chronic alcohol use.
In pneumonia, a very characteristic “currant jelly” sputum is produced. Why does this happen? (Hint: it relates to a colony characteristic.)
Interestingly, two other species are found infrequently:
- Klebsiella ozaenae causes atrophic rhinitis.
- Klebsiella rhinoscleromatis causes granulomas in the nose and upper respiratory tract.
Laboratory diagnosis of Klebsiella infections
Diagnosis is typically done with Gram stain and culture of clinical samples.
On Gram stain:
- The capsule appears as a clear halo around the Gram-negative bacillus.
On culture:
- Colonies are mucoid.
- Colonies are lactose fermenting on MacConkey’s agar and EMB.
- It’s urease positive.