Vision
Vision is the special sense that lets you detect and interpret light stimuli using the eyes.
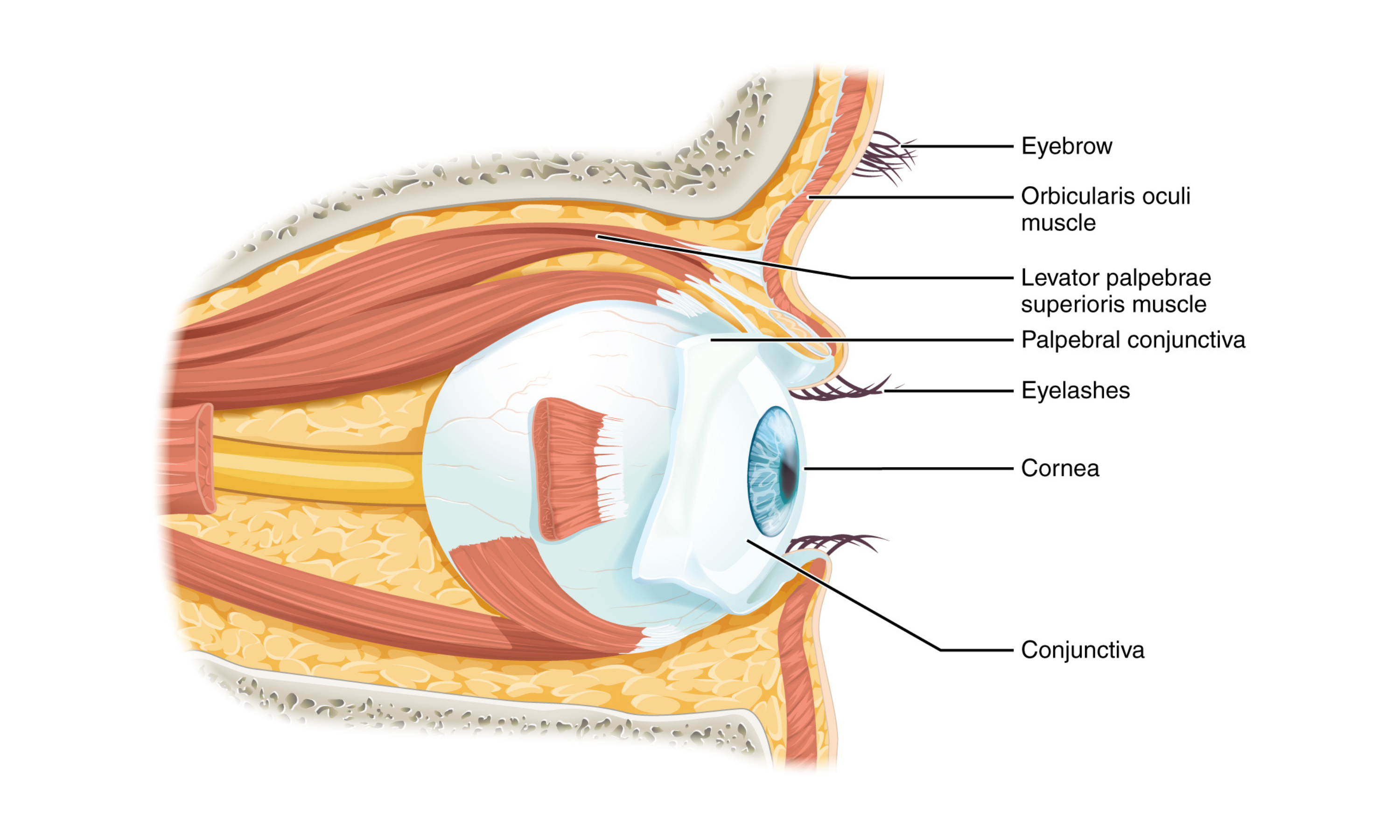
Each eye sits in an orbit of the skull. The orbit’s bony walls help protect the eye and provide attachment points for supportive soft tissues.
Eyelids, with lashes along their edges, help protect the eye from foreign particles.
The inner surface of each eyelid is the palpebral conjunctiva. This membrane continues onto the surface of the eye over the sclera (the “white” of the eye), forming a continuous lining that connects the eyelids to the eyeball.
Tears are produced by the lacrimal gland, located superior and lateral to each eye. Tears then flow through the lacrimal duct toward the medial corner of the eye, helping wash debris from the conjunctiva.
Extraocular muscles
Movement of the eye within the orbit depends on six extraocular muscles. These muscles originate from the orbit’s bones and insert onto the outer surface of the eye:
- Superior rectus, inferior rectus, medial rectus, lateral rectus: Each pulls the eye in the direction suggested by its name (for example, the superior rectus rotates the eye upward).
- Superior oblique: Originates near the posterior orbit, passes through the trochlea (a cartilaginous pulley), and then attaches to the eye at an oblique angle. Contraction rotates the eye laterally.
- Inferior oblique: Originates from the orbit floor and attaches inferolaterally. It also rotates the eye laterally, but it opposes the superior oblique.
Because the eye isn’t perfectly aligned with the sagittal plane, the oblique muscles add a small rotational component when the eye looks up or down.
A seventh muscle, the levator palpebrae superioris, elevates the upper eyelid. It often acts in tandem with the superior rectus when the eye elevates.
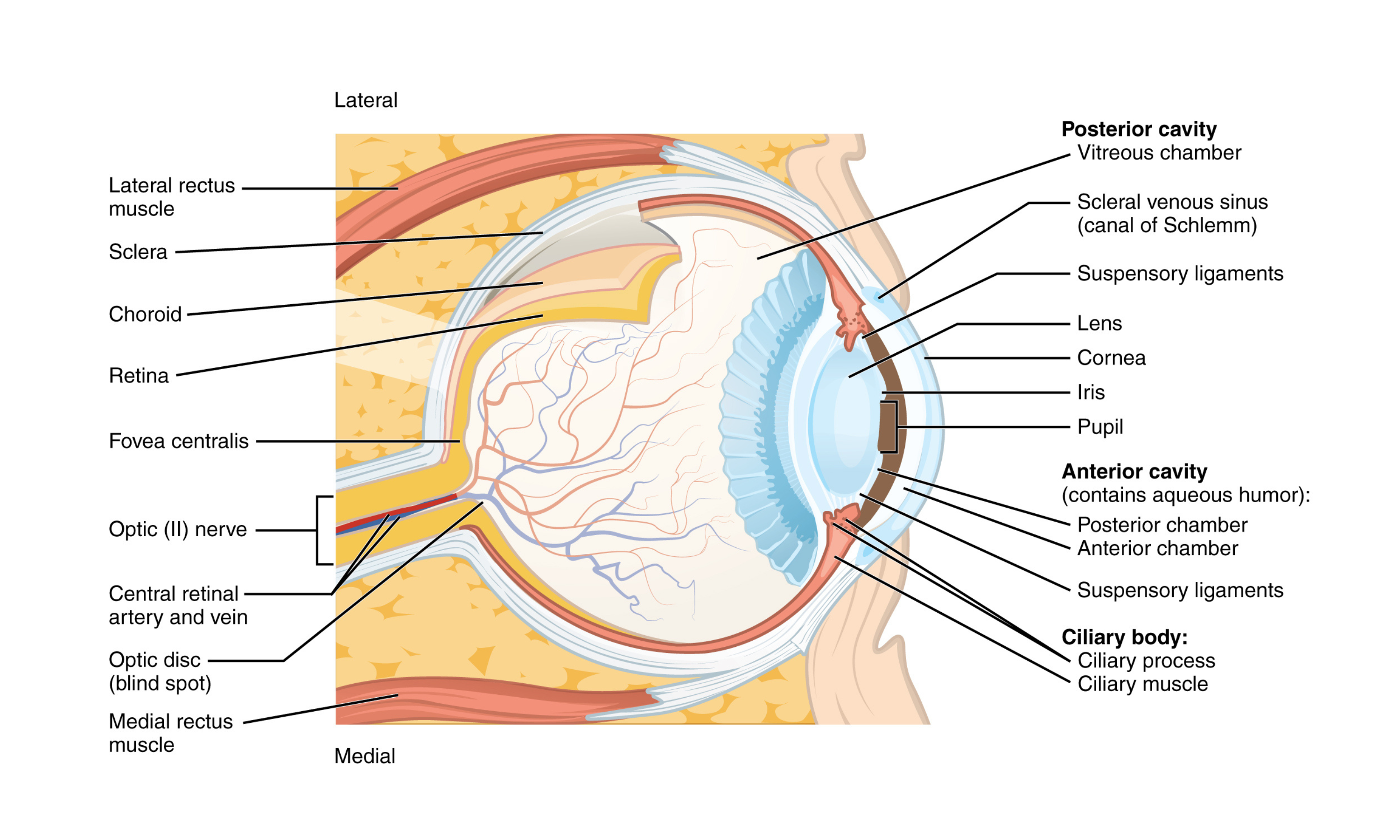
Layers of the eye: The eye is a hollow sphere made of three tunic layers:
- Fibrous tunic: The outermost layer, consisting of the white sclera and the transparent cornea. The cornea covers the anterior tip of the eye and allows light to enter.
- Vascular tunic: The middle layer, made up of the choroid, ciliary body, and iris.
- Choroid: Highly vascular tissue that supplies blood to the eye.
- Ciliary body: Contains muscles connected to the lens by suspensory ligaments (also called zonule fibers). When these muscles contract or relax, they change the lens shape to focus light.
- Iris: The colored part of the eye. Its smooth muscle adjusts the size of the pupil (the central opening) in response to light intensity.
- Neural tunic (retina): The innermost layer containing photoreceptive nervous tissue. It converts light into neural signals.
Retina and photoreceptors
- Within the retina, specialized cells (rods and cones) detect light energy:
- Rods: Contain the pigment rhodopsin in stacked discs; specialized for low-light and peripheral vision.
- Cones: Contain infolded membranes with opsins, sensitive to distinct wavelengths (red, green, blue).
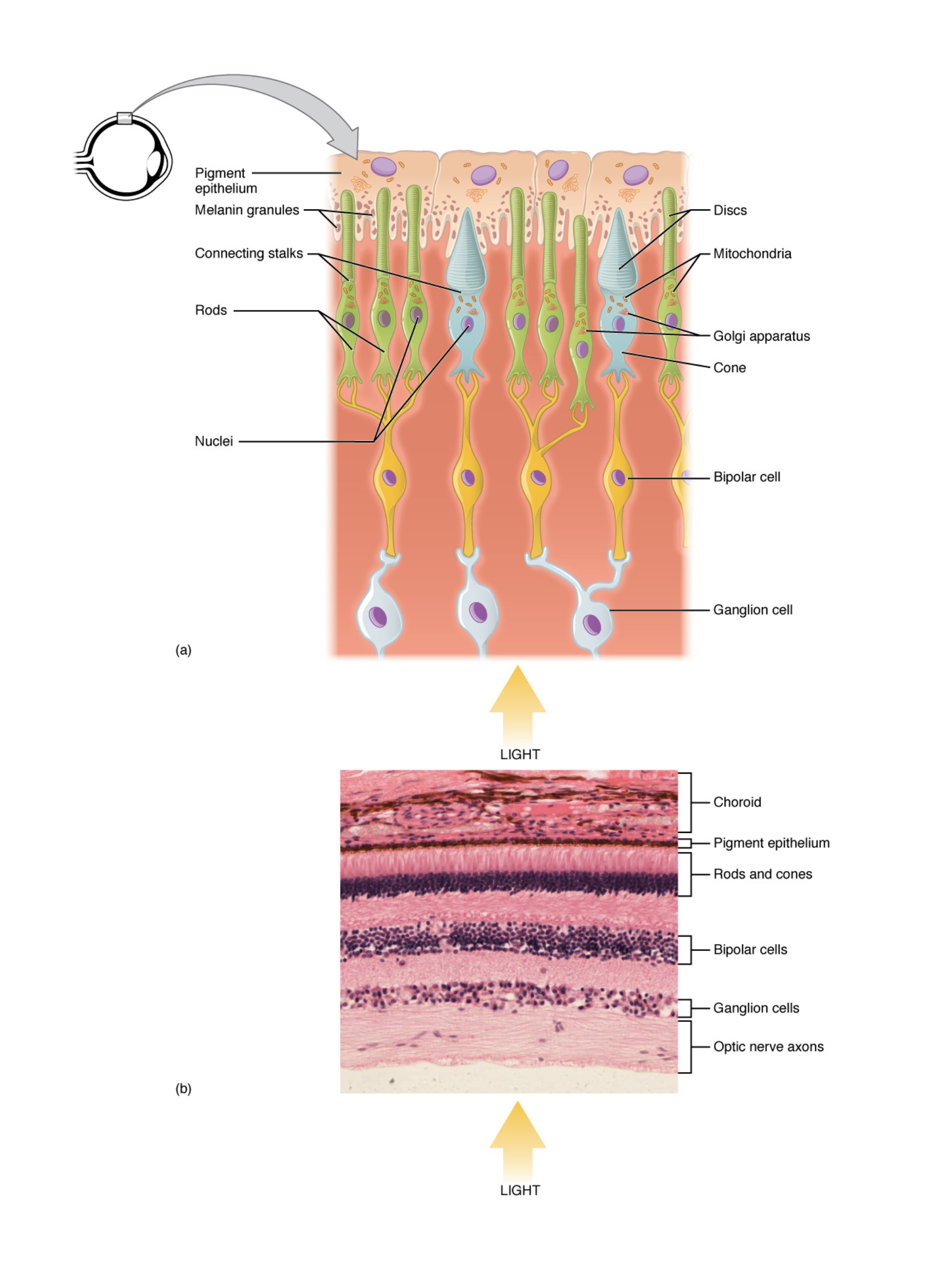
Retinal layers
- Photoreceptors (rods and cones) change their membrane potential in response to light. This changes how much neurotransmitter they release onto bipolar cells.
- Bipolar Cells relay signals to retinal ganglion cells (RGCs), with amacrine cells helping refine and modulate the signal.
- RGCs form the optic nerve at the optic disc, creating a blind spot because this region has no photoreceptors.
At the center of the retina is the fovea. It lacks extra layers and blood vessels, which supports maximum visual acuity. In the fovea, each photoreceptor connects to a single RGC. In more peripheral retina, multiple photoreceptors converge onto fewer RGCs, which reduces fine detail.
Light transduction
- Light triggers chemical changes in rod and cone pigments. This starts a cascade that ultimately changes RGC output. Differences in rod versus cone structure and pigment composition help explain the eye’s ability to detect a wide range of light intensities and colors.
Visual pathway to the brain
- Retina: Detects light through photoreceptors.
- Optic nerve: Carries neural signals from the retina.
- Optic chiasm: Site where some optic nerve fibers cross, supporting binocular vision.
- Optic tracts: Carry visual information to the lateral geniculate nucleus (LGN) of the thalamus.
- Optic radiations: Carry signals to the primary visual cortex (V1) in the occipital lobe.
Visual field processing
- This organization ensures that both brain hemispheres receive input from each eye, which is important for depth perception and binocularity.
Parallel processing
- Magnocellular pathway (magno): Movement and spatial recognition (the “where” pathway).
- Parvocellular pathway (parvo): Color and detail (the “what” pathway).
Dorsal stream (“where”): Identifies location and motion in the parietal lobe.
Ventral stream (“what”): Recognizes shapes and objects in the temporal lobe.
Feature detection and parallel processing
- Neurons in the visual cortex specialize in different stimulus features:
- Simple cells: Edge orientation.
- Complex cells: Motion direction.
- Hypercomplex cells: Complex shapes or specific lengths.
Color detection relies on S-cones (blue), M-cones (green), and L-cones (red). Motion detection involves areas such as the middle temporal region and is supported by the magnocellular pathway.
Clinical correlates
- Damage at specific points along the visual pathway (for example, the optic nerve, optic tract, or occipital lobe) produces characteristic visual field defects (such as homonymous hemianopia). Conditions like visual agnosia (inability to recognize objects) and motion blindness show how these pathways are necessary for normal vision.