Psychological disorders
Approaches in understanding psychological disorders
Biomedical vs. biopsychosocial approaches
- Health psychology looks at how health is shaped by biological, psychological, and sociocultural factors. This integrated perspective is often called the biopsychosocial model.
- Specialists in health psychology work to improve well-being through public policy, education, intervention, and research. For example, they might study how genetics, behavior patterns, relationships, and psychological stress interact to influence health. They may also design methods that encourage positive behavior changes to reduce poor health outcomes.
Classifying psychological disorders
- A psychological disorder (or mental disorder) is a syndrome involving a significant disruption in cognition, emotion regulation, or behavior. This disruption reflects dysfunction in psychological, biological, or developmental processes.
- The disruption typically leads to substantial distress or difficulty in everyday life (for example, in social or occupational settings). Psychopathology is the field that studies these disorders, including their symptoms, causes (etiology), and treatments, as well as how disorders present in individuals.
Because no single definition fits every case, one useful framework is harmful dysfunction. This view treats mental processes (such as cognition, perception, and learning) as internal systems shaped by evolution. A dysfunction occurs when one of these processes fails to operate as it normally should. However, a dysfunction is classified as a disorder only when it also causes harm - judged by cultural standards or by clear distress or impairment in daily life.
In the United States, many practitioners use the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) to classify mental health conditions. It provides detailed descriptions of disorders, diagnostic criteria, prevalence data, and risk factors. The DSM-5 also discusses comorbidity, which is when two or more disorders occur together.
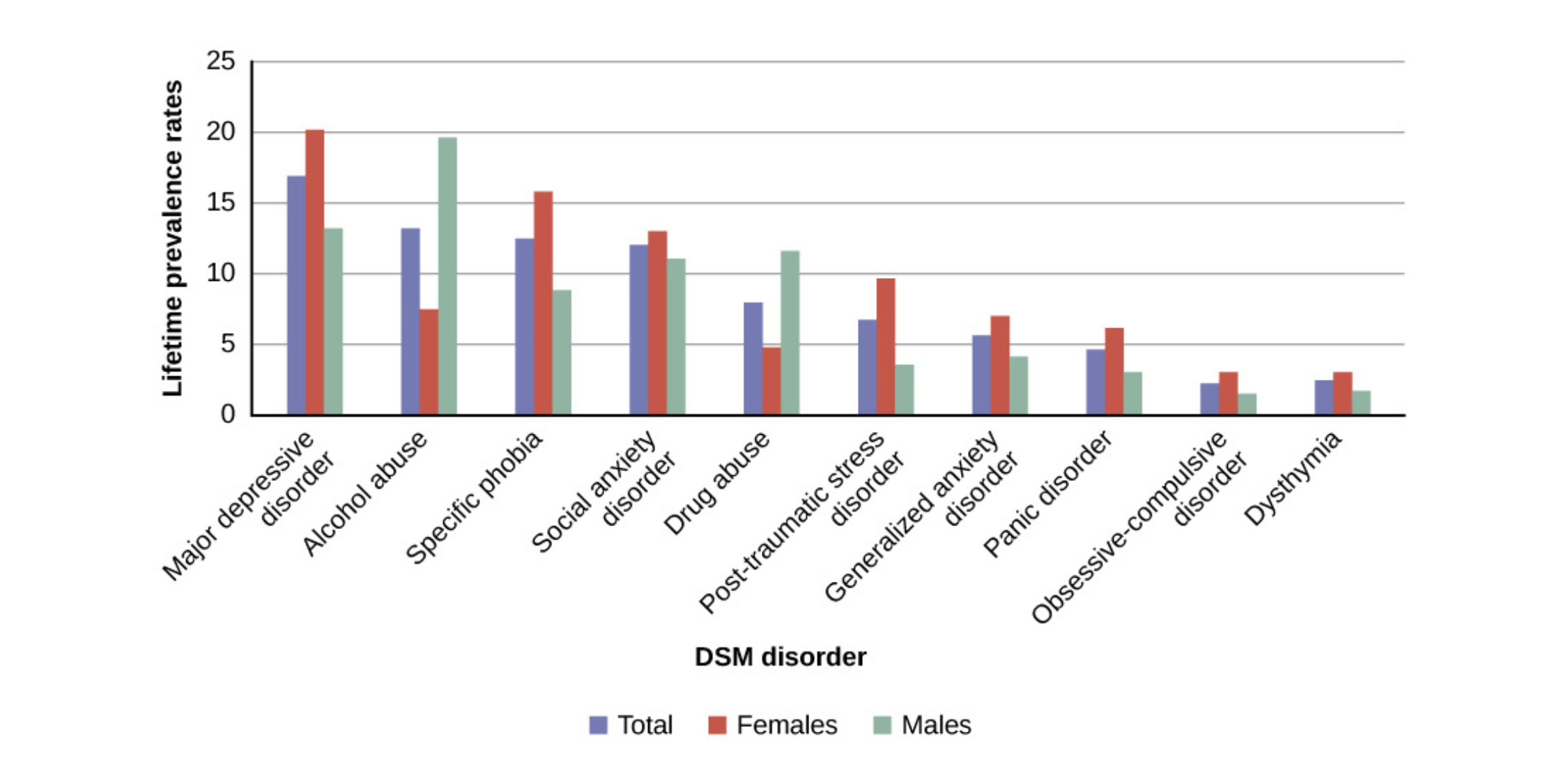
Rates of psychological disorders
Lifetime prevalence rates show how common particular disorders are among adults in the United States, based on a large, nationally representative sample. Many disorders - such as substance use disorders - also commonly occur alongside other forms of mental illness.
Types of psychological disorders
Anxiety
- Anxiety disorders involve excessive and persistent fear or anxiety, along with related disruptions in behavior. Examples include social anxiety disorder, panic disorder, and generalized anxiety disorder. As a group, these are among the most common mental health conditions and are often comorbid with other disorders.
- Social anxiety disorder: Intense fear of negative evaluation in social situations, often leading to avoidance.
- Panic disorder: Recurrent, unexpected panic attacks (sudden surges of extreme fear with strong fight-or-flight symptoms), along with ongoing worry about future attacks or behavior changes aimed at preventing them.
- Generalized anxiety disorder: Chronic, excessive worry about everyday matters, often paired with restlessness, irritability, and difficulties with sleep or concentration.
Obsessive-compulsive disorder (OCD)
- OCD involves intrusive, distressing obsessions (persistent, unwanted thoughts or urges) and/or compulsions (repetitive behaviors or mental acts intended to reduce anxiety). People with OCD may recognize that their thoughts are illogical, but still find them difficult to dismiss.
Trauma- and stressor-related disorders
- Exposure to extremely stressful or traumatic events can lead to disorders such as posttraumatic stress disorder (PTSD).
- Symptoms can include intrusive memories, avoidance of reminders, negative emotional states, and heightened startle responses, lasting for at least one month.
Somatic symptom and related disorders
- These disorders involve physical symptoms that cause significant distress in a person’s thoughts, feelings, and behaviors, but that can’t be explained by other medical or psychological conditions. Examples include hypochondriasis, pain disorder, and conversion disorder.
Bipolar and related disorders
- These disorders involve shifts in mood, ranging from depression to mania. A manic episode is a distinct period of abnormally elevated or irritable mood, along with increased activity or energy. Depression may also occur, but it isn’t required for a bipolar disorder diagnosis.
Depressive disorders
- These disorders are defined by depression as the primary feature. Major depressive disorder involves persistent sadness or loss of interest in usual activities for at least two weeks, often accompanied by changes in appetite, sleep, and cognitive function. Subtypes include seasonal pattern (i.e. winter blues) and peripartum or postpartum (during or after pregnancy) onset.
Schizophrenia
- Schizophrenia is a psychotic disorder involving severe disruptions in thought, perception, emotion, and behavior. Symptoms can include hallucinations, delusions, and disorganized behavior. These symptoms often interfere with everyday functioning.
Dissociative disorders
- Dissociative disorders involve a detachment or split from one’s core sense of self, affecting memory and identity. They include dissociative amnesia, depersonalization/derealization disorder, and dissociative identity disorder (in which two or more distinct personality states emerge).
Personality disorders
- Personality disorders involve pervasive, long-lasting personality styles that differ markedly from cultural expectations and that cause distress and impair relationships. The DSM-5 groups them into:
- Cluster A (odd or eccentric traits), i.e. Paranoid personality disorder, Schizoid personality disorder
- Cluster B (dramatic, emotional, or erratic traits), i.e. Antisocial, Borderline, Histrionic and Narcissistic personality disorders
- Cluster C (nervous or fearful traits), i.e. Avoidant, Dependent and Obsessive-compulsive personality disorders
Biological bases of nervous system disorders
Schizophrenia
- Evidence strongly supports a genetic component. Excess dopamine activity has been linked to schizophrenia, and medications that block dopamine or serotonin receptors can reduce symptoms. Many affected individuals also show structural brain differences, such as enlarged ventricles and reduced gray matter.
Depression
- Mood disorders (including major depressive disorder and bipolar conditions) often run in families, pointing to genetic and biological influences. Brain regions involved in emotional processing and regulation (such as the amygdala and prefrontal cortex) can show abnormal activity. Low levels or imbalances of norepinephrine and serotonin may contribute to depression.
Alzheimer’s disease
- Alzheimer’s disease involves the buildup of amyloid deposits and tau protein, which damages neurons and forms plaques. This damage can lead to severe memory impairment. Risk is increased by genetic susceptibility and by factors such as Down syndrome, type 2 diabetes, hypertension, repeated concussions, and chronic inflammation.
Parkinson’s disease
- Parkinson’s disease primarily affects dopamine-producing neurons in the substantia nigra, often due to deposits of alpha synuclein. Common signs include rigidity, resting tremors, abnormal gait [e.g., shuffling, freezing, festination (short, rapid steps with a forward lean)], slowed movements, and emotional or cognitive changes. Although Parkinson’s is often idiopathic, certain neurotoxins can cause it. Dopamine agonists are one treatment option.
Stem cell-based therapy for CNS regeneration
- Neural stem cells can generate new brain cells, including neurons, astrocytes, and oligodendrocytes. This may help restore function lost in neurodegenerative diseases such as Parkinson’s disease or ALS (Lou Gehrig’s disease).