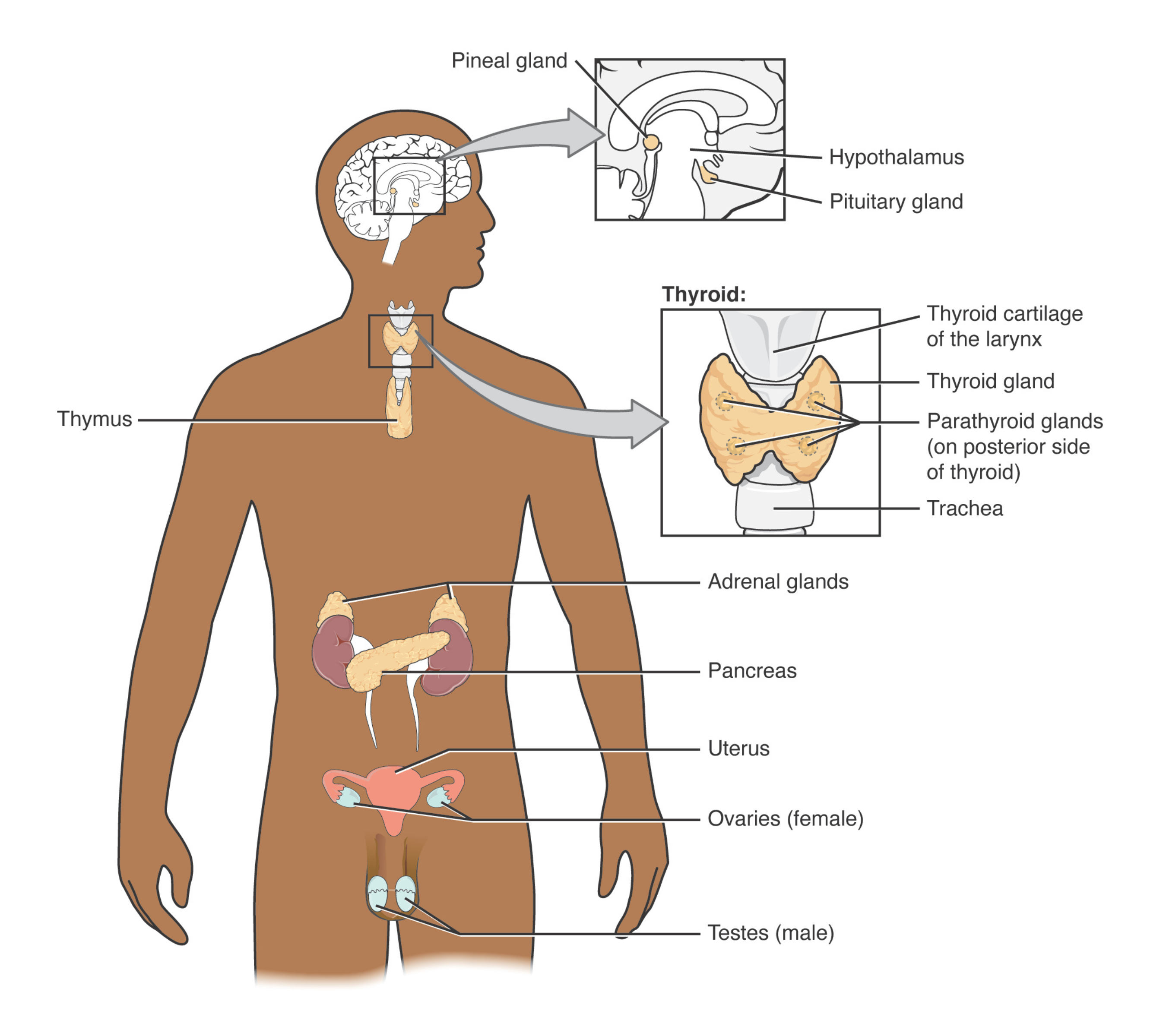
Lipids and the endocrine system
Lipids
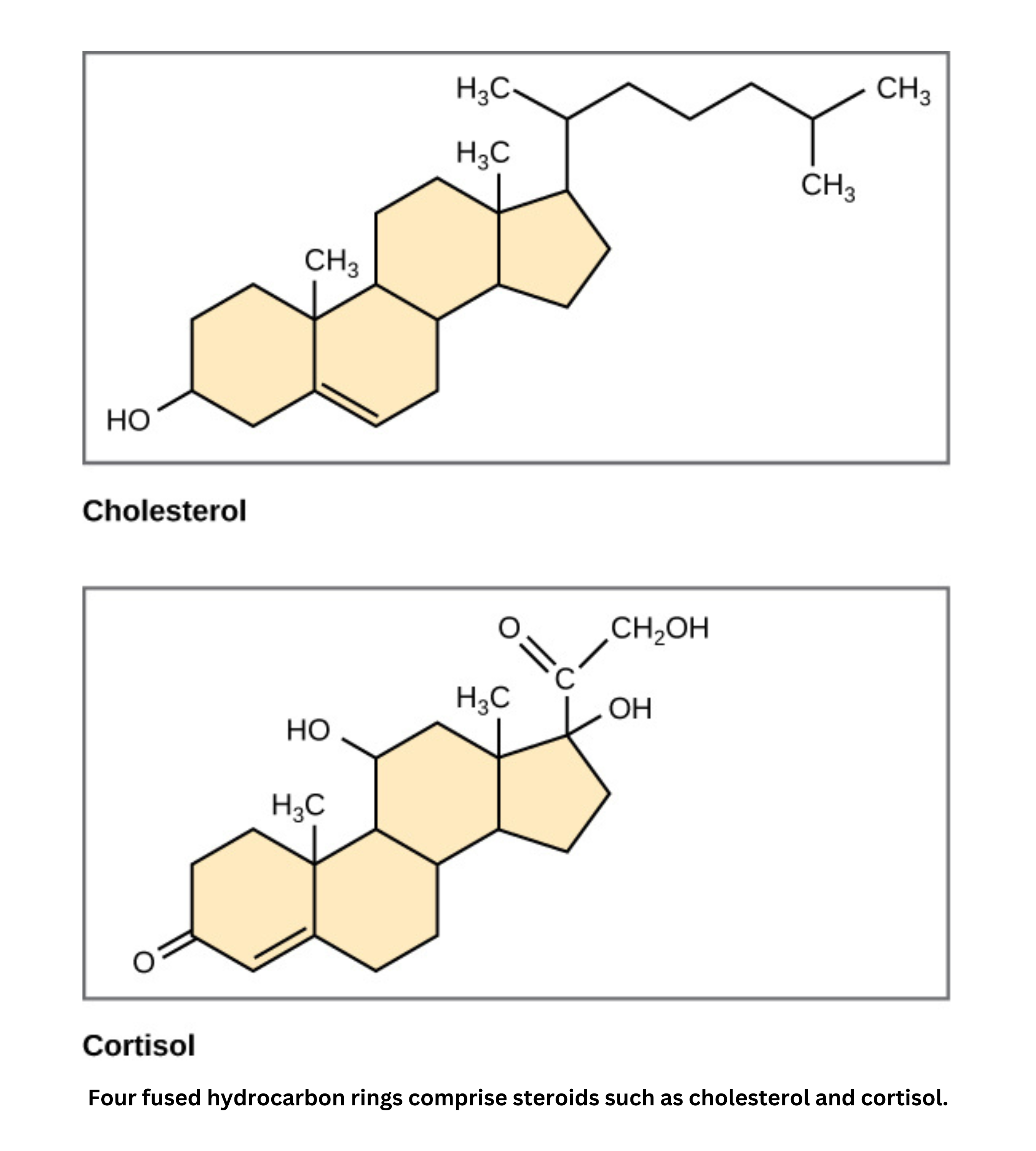
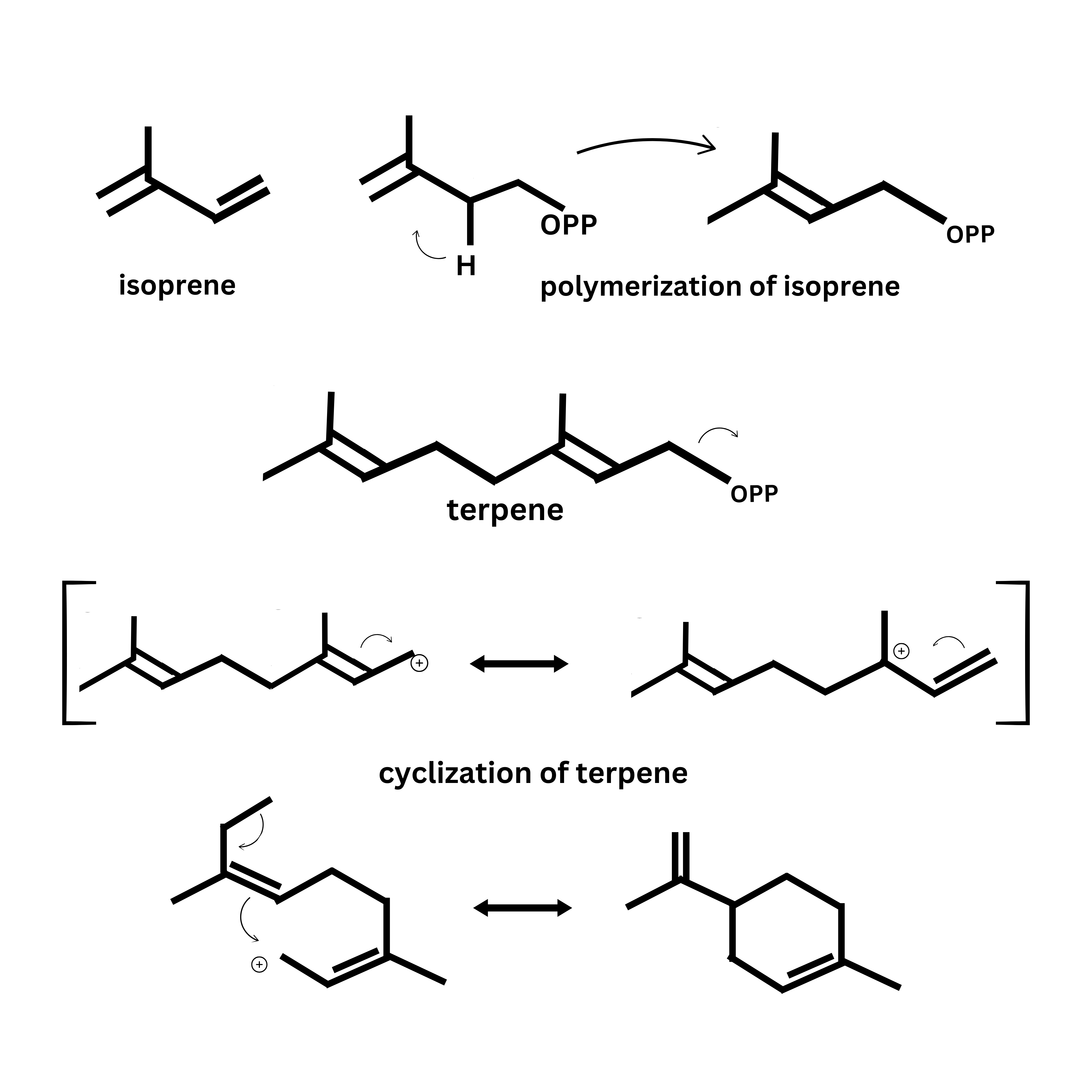
Steroids such as cholesterol, testosterone, and estrogen share a multi-ring structure formed through a complex biosynthetic process. Their synthesis begins with squalene, a triterpene made of six isoprene units. When isoprene units polymerize, they form terpenes. The double bonds in terpenes allow squalene to undergo cyclization, creating the fused-ring core found in steroids.
Terpenes form when isoprene is polymerized. Because they contain double bonds, these molecules can undergo cyclization. Terpenes are classified by the number of isoprene subunits they contain:
- Monoterpenes have 2
- Diterpenes have 4
- Triterpenes like squalene have 6
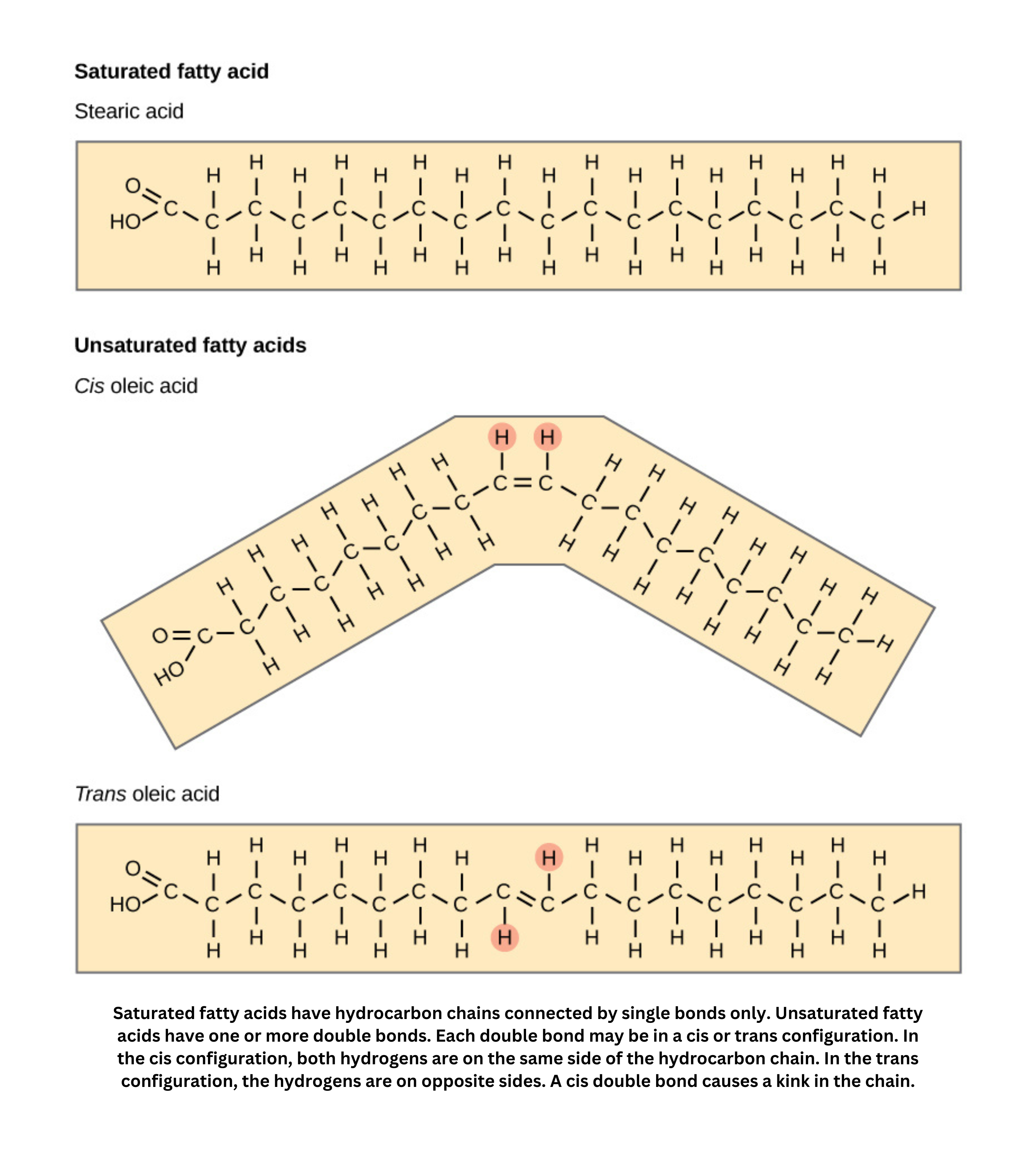
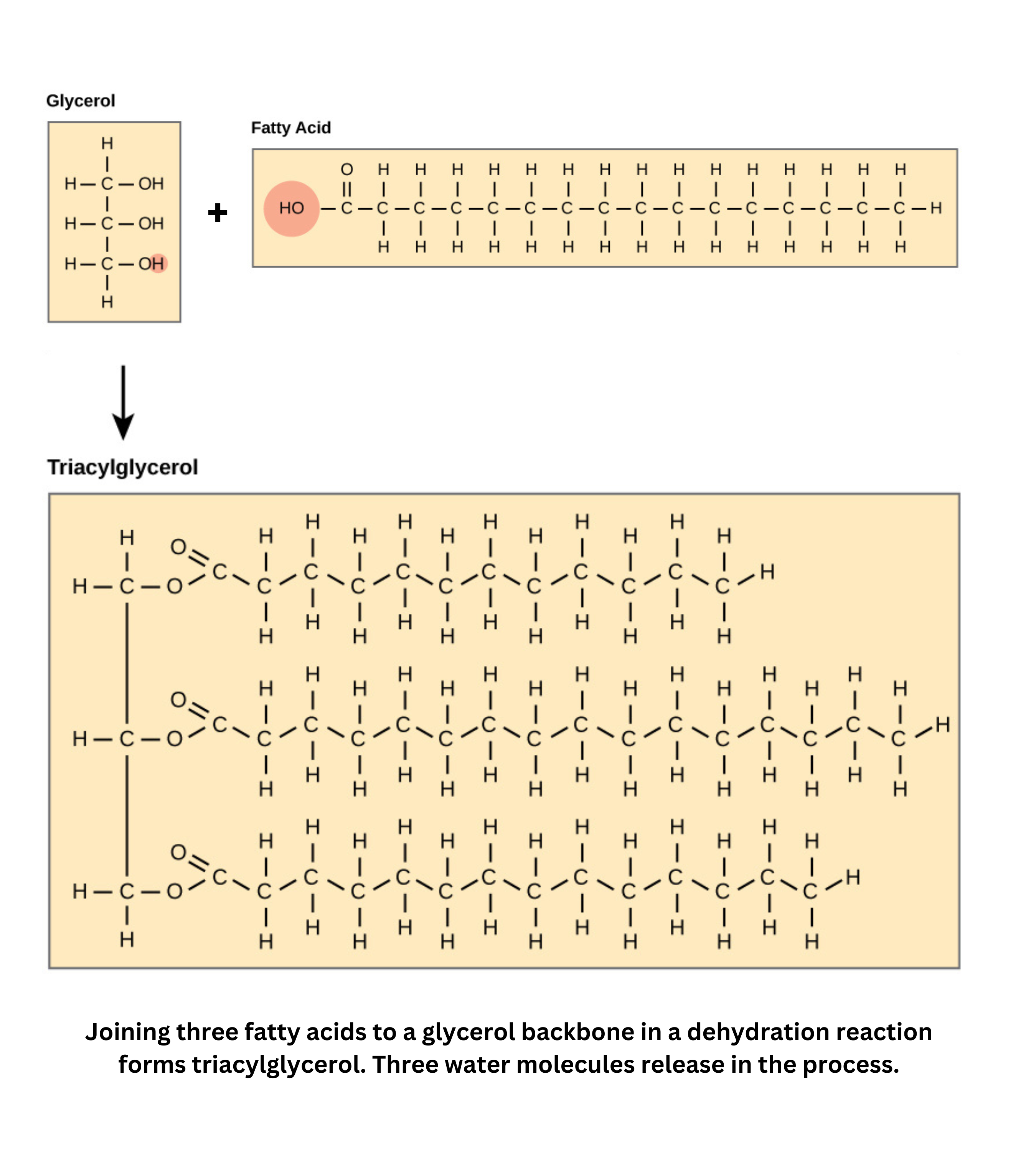
In lipid biochemistry, triacylglycerols (fats) form when three fatty acids esterify with a glycerol molecule. This reaction can be reversed through saponification, which splits fats back into glycerol and free fatty acids. Before further metabolism, fatty acids are activated through phosphorylation and transesterification. Additionally, fatty acid synthesis follows a mechanism similar to a Claisen condensation, showing a common biochemical strategy for building larger molecules from smaller units.
Endocrine system: hormones and their sources
The endocrine system is a chemical control network that helps maintain homeostasis at the cell, tissue, and organ level. It works through hormones released by an endocrine gland, which secretes signaling molecules directly into surrounding fluids (rather than through ducts). Each hormone travels through the bloodstream to act on specific target cells, where it regulates metabolism and function.
In contrast:
- The exocrine system uses ducts to transport non-hormonal secretions (e.g., sweat or digestive enzymes)
- Autocrine signals affect the same cells that secrete them
- Paracrine signals act locally on nearby cells
Major endocrine glands
The pineal gland secretes melatonin, which helps regulate sleep cycles.
The thyroid produces metabolic thyroid hormones (which require iodine) and releases calcitonin, which lowers blood calcium by depositing it into bone.
In contrast, the parathyroid secretes parathyroid hormone (PTH), which raises blood calcium by promoting bone resorption and enhancing calcium uptake.
The thymus secretes factors that support T-cell development.
The adrenal glands produce:
- Epinephrine and norepinephrine for the fight-or-flight response
- Mineralocorticoids like aldosterone to increase sodium and water retention
- Glucocorticoids like cortisol to increase blood sugar during stress
- Androgens that include testosterone
Within the pancreas, glucagon elevates blood sugar (by breaking down glycogen), while insulin lowers blood sugar (by enabling cellular glucose uptake).
The ovary primarily produces estrogen, whereas the testis chiefly secretes testosterone to support male reproductive functions.
The hypothalamus is a key regulator because it produces and releases factors that influence the pituitary gland:
- GnRH (Gonadotropin Releasing Hormone), which stimulates FSH and LH release
- CRF (Corticotropin Releasing Factor)
- TRH (Thyroid Releasing Hormone)
- Dopamine (which inhibits prolactin)
- GHRH (Growth Hormone Releasing Hormone)
The hypothalamus also synthesizes ADH (antidiuretic hormone, also called vasopressin), which increases water reabsorption in the kidneys, and oxytocin, which induces uterine contractions during labor and promotes milk ejection during breastfeeding.
The anterior pituitary gland produces a suite of hormones commonly remembered as FLAT PEG:
- FSH (follicle-stimulating hormone) stimulates ovarian follicles and sperm production
- LH (luteinizing hormone) triggers ovulation and increases testosterone levels
- ACTH (adrenocorticotropic hormone) prompts the adrenal cortex to release corticosteroids
- TSH (thyroid-stimulating hormone) promotes thyroid hormones secretion
- Prolactin supports milk production
- Endorphins help modulate pain
- GH (growth hormone) stimulates growth of muscle and bone while enhancing fat metabolism
The posterior pituitary stores ADH (antidiuretic hormone) and oxytocin produced by the hypothalamus.
Major endocrine pathologies
In diabetes, the body either fails to produce enough insulin or has insulin receptors that do not function properly. In either case, glucose cannot enter cells effectively, leading to high blood sugar. Because cells can’t access glucose for energy, they shift toward fatty acid metabolism, producing ketone bodies. This can lead to ketoacidosis. Excess glucose in the urine also pulls water with it by osmosis, contributing to water loss.
In hypothyroidism, decreased levels of thyroid hormone slow metabolism. When hypothyroidism is caused by an iodine deficiency, the thyroid may enlarge into a goiter due to a buildup of uniodinated hormone precursors.
Conversely, hyperthyroidism involves overproduction of thyroid hormones, which speeds up metabolic processes.
Excess Growth Hormone during childhood can cause Gigantism, characterized by well-proportioned excessive growth. Overproduction later in life leads to Acromegaly, marked by disproportionate growth in regions still responsive to the hormone.
Neuroendocrinology
Neuroendocrinology studies how neurons interact with the endocrine system to regulate bodily functions. A central idea is that electrical signals in neurons can influence the secretion of hormones by endocrine glands.
A key example is the hypothalamus, which sends neural signals to the pituitary gland to control the release of hormones that regulate processes such as growth, metabolism, and stress. These hormonal signals can also affect neural activity, creating feedback loops that help maintain homeostasis. Certain molecules called neuropeptides can act as both neurotransmitters and hormones.
Endocrine system: mechanisms of hormone action
Cellular mechanisms of hormone action describe what happens inside a target cell after a hormone binds its receptor.
Pathways:
- In the cAMP pathway, an amino acid hormone binds its receptor, activating a G protein. The G protein stimulates adenylate cyclase to produce cAMP, which triggers a protein kinase cascade that changes cellular activity.
In the Phospholipid pathway, a similar sequence occurs, but the activated Phospholipase C splits a membrane phospholipid into DAG and IP3. DAG activates another protein kinase cascade, while IP3 releases from the ER.
The Steroid pathway works differently: the hormone crosses the membrane, binds its receptor in the cytoplasm or nucleus, and forms a transcription factor complex that activates specific genes.
Hormone transport and specificity
- Hormones are transported primarily through the bloodstream and lymph, allowing them to act on distant target tissue.
Specificity depends on whether cells have the appropriate receptors, and receptor levels can be upregulated or downregulated. The nervous system can modulate hormone release through feedback control, such as adjusting normal blood glucose set points in response to stress or mood changes caused by low estrogen during menses.
Hormones are regulated through 3 types of stimuli:
- Humoral (directly by blood chemistry)
- Neural (via nerve signals, as in fight or flight)
- Hormonal (via tropic hormones from other glands)