Fungi causing superficial mycoses
This section includes cutaneous and subcutaneous mycoses. Cutaneous mycoses are fungal infections of the skin, hair, and/or nails.
Dermatophytes
Dermatophytes can be classified as:
- Trichophyton: infects skin, hair, and nails
- Microsporum: infects only skin and hair
- Epidermophyton: infects only skin and nails
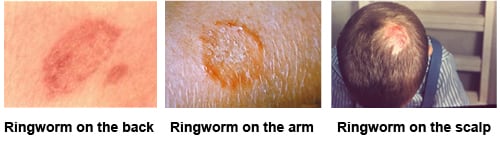
Clinical features of dermatophytosis: Dermatophytes infect dead, keratinised tissue and secrete keratolytic enzymes, which contributes to pathogenicity. The erythematous, itchy rash seen in ringworm (tinea) infections is due to this mechanism. Lesions are typically scaly, itchy, erythematous, and well demarcated. The following types are seen:
- Tinea corporis: on non-hairy skin.
- Tinea pedis/ Athlete’s foot: interdigital area, foot.
- Tinea cruris: groin area.
- Tinea barbae: on bearded areas of the face.
- Tinea faciei: on skin of the face excluding the bearded area.
- Tinea capitis: on the scalp; may become inflammatory. Hair loss and prominent scales may be seen.
- Tinea imbricata: concentric rings of scaling and rash are seen, caused by Tinea concentricum.
- Tinea unguium/ Onychomycosis: nail plates are involved; the nail looks white, opaque, thick, and brittle.
Laboratory diagnosis of dermatophytoses: Diagnosis is done using a KOH preparation of skin, nail, or hair. KOH dissolves keratin so fungal elements can be seen clearly. The smear shows branching, septate hyphae. Fungal culture is done on Sabouraud’s agar or Dermatophyte Test Medium (DTM). Growth on DTM shows red colonies. Wood’s lamp examination may help in a few cases. The table below shows Wood’s lamp findings in superficial mycoses.
| Fungus type | Fluorescence seen |
| Tinea versicolor/ Malassezia furfur | yellowish-white or copper-orange |
| Pityrosporum folliculitis | bluish-white in a follicular pattern. |
| most Microsporum species | blue-green |
| Microsporum gypseum | dull yellow |
| Trichophyton schoenleinii | dull blue |
Tinea versicolor
Also known as Pityriasis versicolor, this is a chronic infection of the skin caused by Malassezia furfur / Pityrosporum orbiculare. It presents as hypopigmented (rarely hyperpigmented), well demarcated, non-inflammatory, sometimes itchy patches. These are commonly seen on the face, neck, torso, and upper body. Laboratory diagnosis is done by:
- Wood’s lamp examination showing yellow fluorescence
- KOH films from skin scrapings showing the characteristic “banana and grape” or “spaghetti and meatballs” appearance
Sporothrix schenckii
Sporothrix schenckii causes a granulomatous infection of the skin and subcutaneous tissue called sporotrichosis (Rose gardener’s disease), since infection often follows a thorn prick. It is a dimorphic fungus.
It presents as a small, firm, violaceous nodule on the skin, followed by nodules along the draining lymphatics, or as ulcerative, suppurative lesions. Rarely, in immunocompromised individuals, it may cause pneumonitis from inhalation of conidia (spores).
- KOH smear is usually negative.
- Histopath examination of skin biopsy samples shows yeast forms and cigar-shaped budding with eosinophilic rays surrounding it, called asteroid bodies.
- Culture shows cream or tan colonies. On microscopy, these show thin hyphae and flower-like clusters of conidia resembling daisy flowers.