Antivirals
Antivirals kill viruses or slow their growth. Only a limited number of viral illnesses have effective antiviral treatment, including influenza (flu), COVID-19, RSV, HBV, HIV, and HSV.
Viruses rely on human enzymes and cellular organelles to survive and multiply. Because of this, most antivirals work by:
- inhibiting a specific viral enzyme needed for replication, or
- blocking the virus from attaching to and entering human cells
Drugs used in the treatment of influenza: Viruses that cause influenza include influenza A, B, and C. Influenza A causes the most severe infections and is responsible for pandemics.
To be effective, influenza antivirals must be started within 48 hours of symptom onset.
Antivirals for influenza include oseltamivir (Tamiflu), zanamivir (Relenza), peramivir (Rapivab), and baloxavir (Xofluza).
- Oseltamivir, zanamivir, and peramivir inhibit a viral enzyme called neuraminidase.
- Baloxavir inhibits viral endonuclease, which stops viral transcription and replication.
Key administration points:
- Baloxavir is given as a single dose.
- Zanamivir is inhaled.
- Peramivir is given intravenously.
Adverse effects include diarrhea, nausea, neutropenia, elevated glucose, elevated liver enzymes, and hypersensitivity.
Drugs used in the treatment of Herpesviral infections: Herpesviruses include HSV 1 and 2, Varicella Zoster Virus (VZV), and Cytomegalovirus (CMV). They cause diseases such as oral and genital herpes, chicken pox, herpes zoster, and infectious mononucleosis.
Acyclovir (Sitavig, Zovirax), valacyclovir (Valtrex), and famciclovir (Famvir) are commonly used to treat HSV 1 and 2 infections.
- Mechanism: They stop viral replication by inhibiting viral DNA polymerase.
Adverse effects include nausea, headache, malaise, renal insufficiency, bleeding tendency, and encephalopathy.
Ganciclovir (Cytovene) is used to treat retinal inflammation caused by CMV.
Drugs used in the treatment of Hepatitis B and C: Hepatitis B and C viruses can cause chronic liver disease.
Drugs commonly used in the treatment of hepatitis B include tenofovir (Viread, Vemlidy), entecavir (Baraclude), adefovir (Hepsera), and lamivudine (Epivir-HBV, Zeffix, Heptodin).
Most antivirals need to be taken for at least one year.
- Mechanism: These are nucleoside or nucleotide analogues that inhibit the HCV enzyme known as RNA-dependent DNA polymerase or reverse transcriptase that helps in viral replication.
Adverse effects include muscle weakness or myopathy, neuropathy, lactic acidosis, mitochondrial dysfunction, and liver dysfunction.
- Adefovir may cause kidney dysfunction.
- Tenofovir may cause renal dysfunction and a decrease in bone density.
Hepatitis C is typically treated with combination antiviral therapy to prevent resistance and attain a cure. They include ribavirin (Rebetol), sofosbuvir (Sovaldi), elbasivir plus grazoprevir (Zepatier), glecaprevir plus pibrentasvir (Mavyret), sofosbuvir plus ledipasvir (Harvoni), sofosbuvir plus velpatasvir (Epclusa), and sofosbuvir plus velpatasvir and voxelaprevir (Vosevi).
Adverse effects include headache, fatigue, diarrhea, and sleep disturbances.
Interferons like interferon alfa (Intron A) and pegylated interferon alpha (Pegasys, PegIntron) are used in the treatment of hepatitis B and C.
- Interferons are naturally occurring immune mediators.
They can cause flu-like symptoms, depression, arrhythmias, tachycardia, and dysfunction of the kidney, heart, liver, thyroid, and bone marrow.
Drugs used in the treatment of HIV and AIDS: Human immunodeficiency virus (HIV) reduces immunity by decreasing levels of CD4 cells, a type of white blood cell.
The most severe form of HIV infection is AIDS or Acute Immunodeficiency Syndrome.
HIV therapy uses combination antiviral therapy to keep viral counts under control and prolong life expectancy. This approach is called HAART (“highly active antiretroviral therapy”). Anti-HIV drugs are classified as follows -
Nucleoside or nucleotide reverse transcriptase inhibitors or NRTIs: They include abacavir (Ziagen), didanosine (Videx), lamivudine (Epivir), stavudine (Zerit), zidovudine (Retrovir), emtricitabine (Emtriva), and tenofovir (Viread).
- Mechanism: They inhibit viral reverse transcriptase enzymes and viral replication.
Adverse effects include peripheral neuropathy, lactic acidosis, myelosuppression, anemia, lipodystrophy, and renal failure.
- Abacavir may cause hypersensitivity reactions.
- Didanosine may cause pancreatitis and liver dysfunction.
Non-nucleoside reverse transcriptase inhibitors or NNRTIs: They include nevirapine (Viramune), efavirenz (Sustiva), delavirdine (Rescriptor), rilpivirine (Edurant), doravirine (Pifeltro), and etravirine (Intelence).
- Mechanism: They inhibit viral reverse transcriptase enzymes and viral replication.
Adverse effects include skin rash, Stevens-Johnson syndrome, hepatitis, liver failure, prolongation of QTc, and delusions.
Protease inhibitors or PIs: They include indinavir (Crixivan), darunavir (Prezista), atazanavir (Reyataz), nelfinavir (Viracept), and tipranavir (Aptivus).
- Mechanism: They inhibit HIV protease, which is essential for viral maturation.
Adverse effects include metabolic syndrome, insulin resistance, lipodystrophy, dyslipidemia, coronary artery disease, and stroke.
- Indinavir may cause kidney stones.
Integrase strand transfer inhibitors or INSTI: They include dolutegravir (Tivicay), elvitegravir (Vitekta), cabotegravir (Apretude, Vocabria), and raltegravir (Isentress).
- Mechanism: They inhibit integration of viral DNA with the host DNA.
Adverse effects are dizziness, depression, sleep disorders, myopathy, and rhabdomyolysis.
Capsid inhibitors: They interfere with the HIV capsid, a protein shell that protects HIV’s genetic material and enzymes needed for replication.
Most commonly used is lenacapavir (Sunlenca).
CCR5 Antagonists: They block the CCR5 coreceptor on the surface of certain immune cells, such as CD4 T lymphocytes (CD4 cells), and prevent HIV from entering the cell.
Maraviroc (Selzentry) is the most common one.
Fusion inhibitors: They block the HIV envelope from merging (fusing) with the host CD4 cell membrane and therefore prevent HIV from entering the CD4 cell.
Enfuvirtide (Fuzeon) is commonly available.
Attachment inhibitors: They block gp120 and prevent HIV from entering the cells.
Fostemsavir (Rukobia) is available.
Postattachment inhibitors: They bind to the CD4 receptor and block HIV from entering the cell.
Ibalizumab (Trogarzo) is available.
Combination anti-HIV drugs: Many anti-HIV drugs are sold as combinations of two or three drugs from either the same or different drug class. Common HIV combination pills are below -
| Brand name | Combination |
|---|---|
| Epzicom | Abacavir + lamivudine |
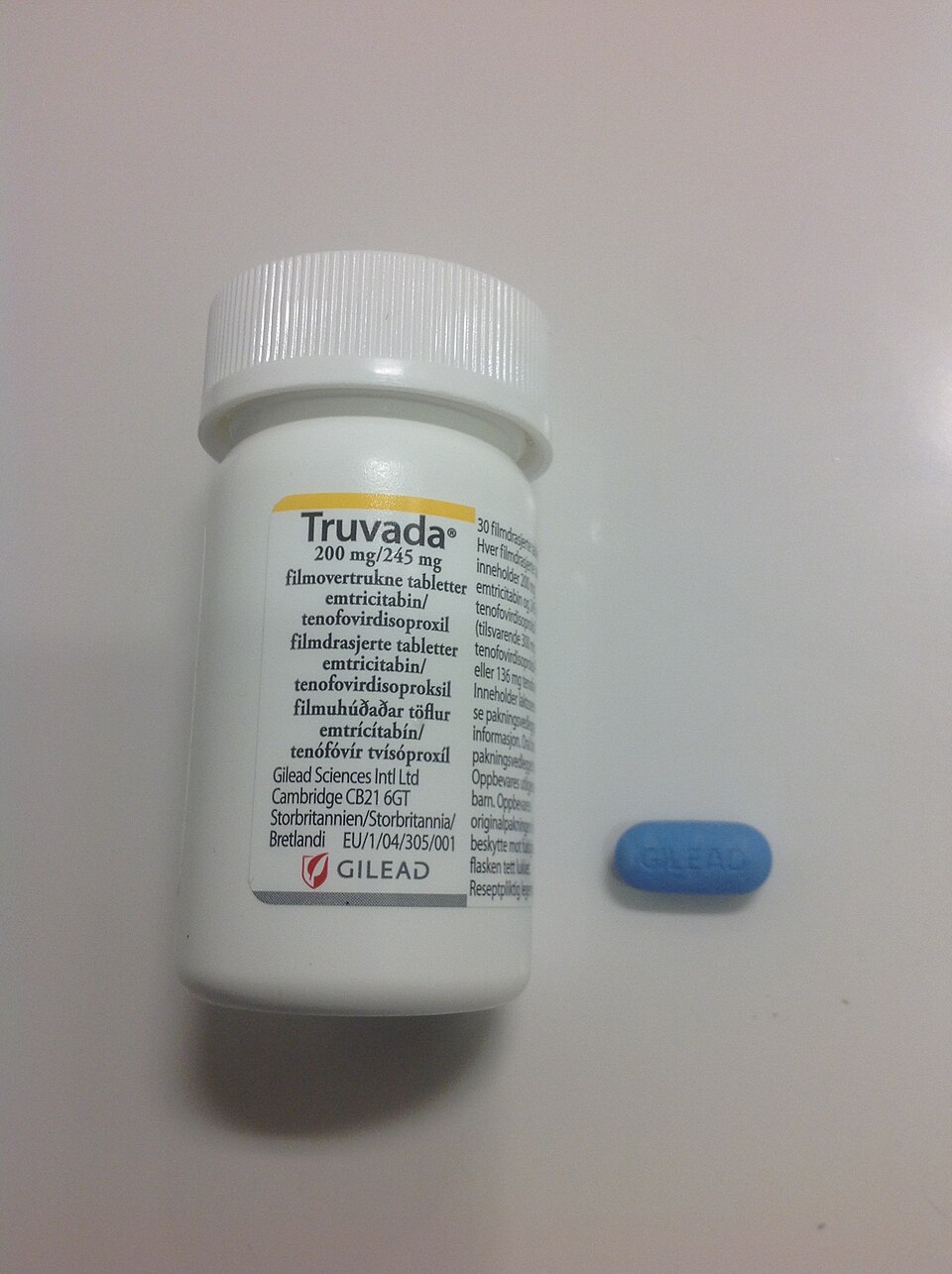
| Descovy, Truvada | Tenofovir + emtricitabine |
| Combivir | Zidovudine + lamivudine |
| Kaletra | Lopinavir + ritonavir |
| Temixys | Lamivudine + tenofovir |
| Biktarvy | Tenofovir + emtricitabine + bictegravir |
| Atripla | Efavirenz + emtricitabine + tenofovir |
| Triumeq | Abacavir + dolutegravir + lamivudine |
Currently, three medications are FDA-approved for pre-exposure prophylaxis (PrEP) for HIV: Truvada, Descovy, and the injectable drug Apretude.
Post-exposure prophylaxis (PEP) is started as soon as possible (and at least within the first 72 hours after exposure) and continues for one month. Combination therapy with Truvada/Descovy or their generics with either one of raltegravir, dolutegravir, darunavir, or ritonavir is recommended for PEP.
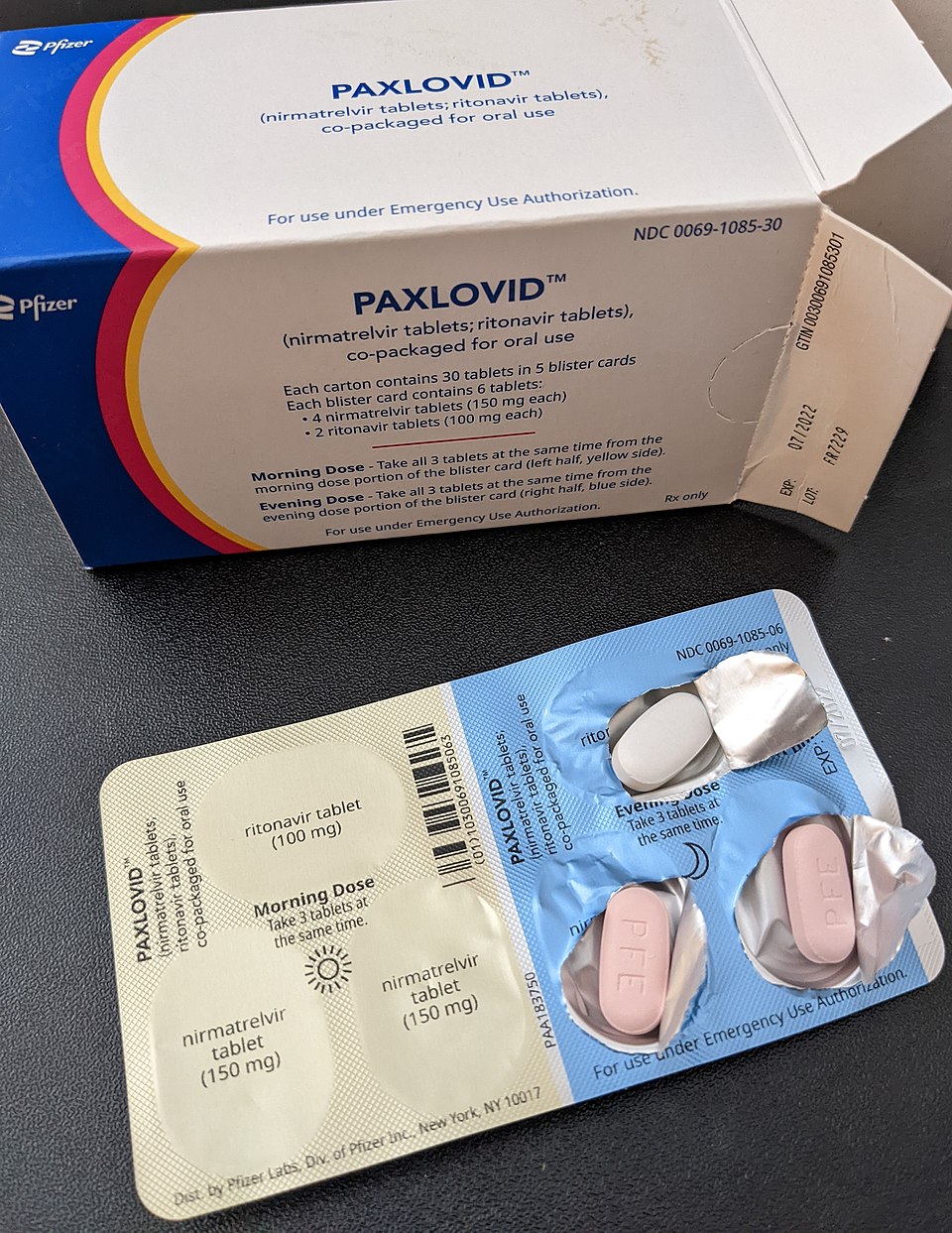
Antivirals used in the treatment of COVID-19: Several newly developed and older antivirals are available to treat COVID-19. These include nirmatrelvir plus ritonavir (PAXLOVID), remdesivir (Veklury), and molnupiravir (Lagevrio).
PAXLOVID inhibits viral replication. It can interact with other medications such as statins, diuretics, antiarrhythmics, antiepileptics, and St. John’s Wort.
Paxlovid adverse effects include metallic taste, diarrhea, headache, nausea, and abdominal pain.
Remdesivir inhibits viral replication by inhibiting viral RNA polymerase.
- Administration: It is administered intravenously.
- Adverse effects include nausea and elevated liver enzymes.
Molnupiravir induces errors in viral replication, which leads to the formation of non-infectious virus.
Adverse effects include diarrhea, rash, and dizziness.
Antivirals used in the treatment of RSV: RSV (Respiratory Syncytial Virus) can cause serious upper and lower respiratory tract infections in infants and older adults.
Ribavirin (Copegus, Moderiba, RibaPak, RibaTab) is used to treat RSV infections. The inhaled version is called Virazole.
Adverse effects include nausea, fever, low blood cell counts, anemia, fatigue, and mood changes.
For patients at high risk of RSV infections (for example, immunocompromised patients and those with lung diseases), palivizumab (Synagis) is given intramuscularly as a preventive measure.
- Palivizumab is a monoclonal antibody that provides passive immunity by binding to the RSV envelope and preventing it from infecting the host.
Adverse effects include rash, sore throat, runny nose, low platelet count, nausea, and diarrhea.
Antimycobacterials: Antimycobacterials are antibiotics that are effective against the bacteria that cause tuberculosis and leprosy.
They include isoniazid, ethambutol, rifampin, pyrazinamide, rifapentine, streptomycin, and moxifloxacin. Bedaquiline and linezolid are used in drug-resistant tuberculosis.
Adverse effects include nausea, liver dysfunction (isoniazid, rifampin, pyrazinamide), reddish discoloration of body fluids and urine (rifampin), visual changes (ethambutol), dizziness, renal toxicity, deafness, and peripheral neuropathy.
Vitamin B6 (pyridoxine) is taken along with isoniazid to prevent peripheral neuropathy.
Multi-drug therapy is administered for a period of 4 -9 months.
Dapsone is used to treat leprosy.