Antiplatelets, anticoagulants and thrombolytics
Antiplatelets
Antiplatelet drugs reduce the ability of platelets to stick together (aggregate). This helps prevent clot formation and lowers the risk of heart attacks and strokes. Based on how they work, antiplatelets can be divided into the classes below.
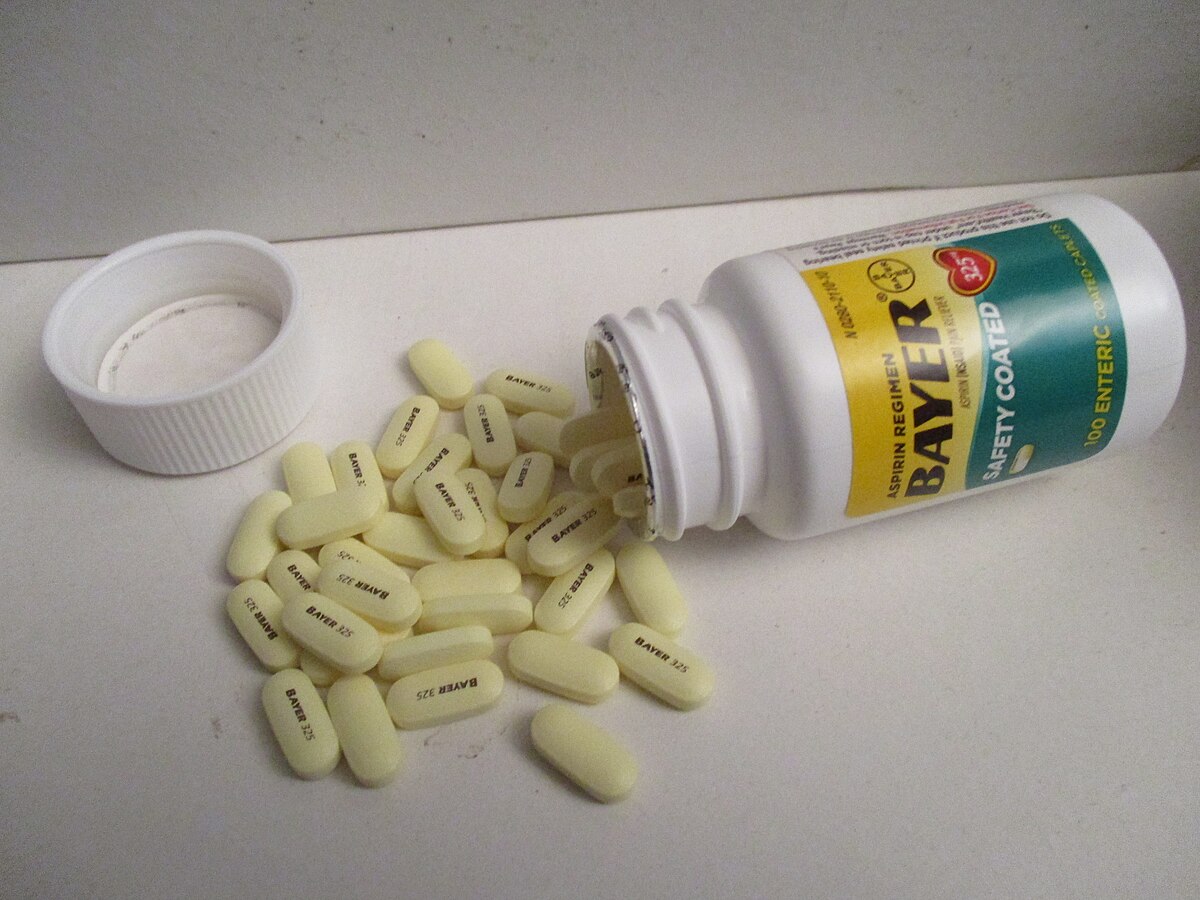
Cyclooxygenase inhibitors: These drugs inhibit the enzyme cyclooxygenase 1 (COX-1). This lowers thromboxane A2 levels, which reduces platelet aggregation (platelet “clumping”). Examples include aspirin (Ecotrin, acetylsalicylic acid) and triflusal (Aflen, Disgren). Adverse effects include nausea, heartburn, abdominal pain, and bleeding. Aspirin is typically stopped 72 hours before planned surgery because it can increase bleeding risk. Aspirin is available over the counter in various doses, such as 81 mg and 325 mg. Low-dose aspirin is also called “baby aspirin.” Aspirin isn’t recommended in children because it can cause potentially fatal Reye’s syndrome, which is associated with liver failure.
ADP P2Y12 inhibitors: These drugs inhibit the ADP (P2Y12) receptor on platelets, which reduces platelet aggregation. ADP is a chemical produced in the body that plays an essential role in clot formation. Examples include clopidogrel (Plavix), prasugrel (Effient), ticlopidine (Ticlid), and ticagrelor (Brilinta). Common side effects include diarrhea and skin rash. Clopidogrel plus aspirin is commonly prescribed in patients with coronary, carotid, and coronary stents.
GPIIb/IIIa inhibitors: The GPIIb/IIIa receptor plays a pivotal role in platelet aggregation. Inhibitors include abciximab (ReoPro), eptifibatide (Integrilin), and tirofiban (Aggrastat). Adverse effects include bleeding and thrombocytopenia.
Phosphodiesterase inhibitors: These drugs increase cAMP levels in platelets, which reduces platelet aggregation. Examples include cilostazol (Pletal) and dipyridamole (Persantine). Adverse effects include headache, nausea, diarrhea, palpitations, and bleeding.
Protease activated receptor-1 (PAR -1) antagonists: These are a newer type of antiplatelet drug. They reduce platelet activation by blocking PAR-1 receptors, which blocks the action of the clotting factor thrombin on platelets. Vorapaxar (Zontivity) has been approved by the FDA. Adverse effects include headache, fatigue, nausea, and rash.
Anticoagulants
Anticoagulants reduce the blood’s ability to clot. Indications overlap with antiplatelets, and anticoagulants are also used to prevent and treat clots in atrial fibrillation, pulmonary embolisms, and peripheral artery disease. They are classified as follows.
Warfarin: Warfarin prevents the synthesis of vitamin K-dependent clotting factors by inhibiting the enzyme epoxide reductase. It’s sold under the brand names Coumadin and Jantoven. Patients taking warfarin need monitoring with a blood test called PT/INR, which measures prothrombin time. Warfarin shouldn’t be used in pregnancy because it’s teratogenic. The most common adverse effect is bleeding, especially internal bleeding. Warfarin has many drug and food interactions, including with antiplatelet drugs, alcohol, NSAIDs, grapefruit juice, and green leafy vegetables. Bleeding due to warfarin overdose can be reversed with vitamin K. The full therapeutic effect of warfarin takes three to five days.
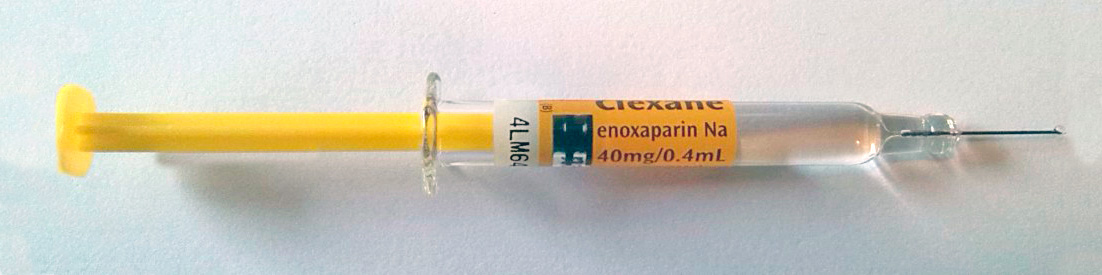
Heparin: Heparin enhances the activity of antithrombin III, which then inhibits clotting factors such as thrombin, factor IX, and factor X. It comes in two forms: unfractionated heparin (UFH) and low molecular weight heparin (LMWH). Unfractionated heparin is available as generic heparin sodium injection for intravenous or subcutaneous use. Types of LMWH include enoxaparin (Lovenox), dalteparin (Fragmin), and tinzaparin (Innohep). LMWHs are derived from UFH, have a longer half-life, and have more predictable effects than UFH. Heparins are used to prevent and treat blood clots in heart attacks, stroke, pulmonary embolism, and deep vein thrombosis (DVT). The most common adverse effect is bleeding. LMWH dosing must be reduced in patients with renal failure. Heparin may rarely cause thrombocytopenia (low platelets) and decreased bone density (osteopenia). Heparin must be monitored with aPTT (activated partial thromboplastin time) or anti-Xa levels. Bleeding can potentially be reversed with protamine, a heparin antagonist that forms a complex with heparin.
Factor Xa inhibitors: These anticoagulants inhibit the function of clotting factor Xa, either directly or indirectly. Examples include apixaban (Eliquis), rivaroxaban (Xarelto), fondaparinux (Arixtra), and edoxaban (Savaysa). Adverse effects include bleeding and thrombocytopenia.
Direct thrombin inhibitors: These drugs directly inhibit thrombin, a key clotting factor in blood clot formation. Important examples include argatroban, bivalirudin (Angiomax), and dabigatran (Pradaxa). Dabigatran is the only oral drug in this class; the others are injectable. They can be used as substitutes for heparin. The main adverse effect is bleeding.
Warfarin and heparin are traditional anticoagulants. DOACs (direct oral anticoagulants) are taken orally and don’t require regular blood testing or special diets like warfarin, and they have fewer adverse effects. DOACs include the direct thrombin inhibitor dabigatran and factor Xa inhibitors such as rivaroxaban, apixaban, and edoxaban.
Thrombolytics
Thrombolytics (also called fibrinolytics) break down existing blood clots. They work by activating plasmin, an enzyme that dissolves clots. Commonly used thrombolytics include alteplase (Activase), reteplase (Retavase), and tenecteplase (TNKase). They can be used to treat conditions such as heart attacks (myocardial infarction), pulmonary embolism, and stroke. Adverse effects include bleeding and allergic reactions. They’re contraindicated in recent surgery, active bleeding, recent brain injury, and severe hypertension.